p53 deficiency enhances the efficiency of somatic cell reprogramming to a pluripotent state. As p53 is usually mutated in human tumors and many mutated forms of p53 gain novel activities, we studied the influence of mutant p53 (mut-p53) on somatic cell reprogramming. Our data indicate a novel gain of function (GOF) property for mut-p53, which markedly enhanced the efficiency of the reprogramming process compared with p53 deficiency. Importantly, this novel activity of mut-p53 induced alterations in the characteristics of the reprogrammed cells. Although p53 knockout (KO) cells reprogrammed with only Oct4 and Sox2 maintained their pluripotent capacity in vivo, reprogrammed cells expressing mutant p53 lost this capability and gave rise to malignant tumors. This novel GOF of mut-p53 is not attributed to its effect on proliferation, as both p53 KO and mut-p53 cells displayed similar proliferation rates. In addition, we demonstrate an oncogenic activity of Klf4, as its overexpression in either p53 KO or mut-p53 cells induced aggressive tumors. Overall, our data show that reprogrammed cells with the capacity to differentiate into the three germ layers in vitro can form malignant tumors, suggesting that in genetically unstable cells, such as those in which p53 is mutated, reprogramming may result in the generation of cells with malignant tumor-forming potential.
Reprogramming of differentiated adult cells into their embryonic state was demonstrated when oocytes implanted with nuclei of adult somatic cells gave rise to viable animals (Wilmut et al., 1997). However, the understanding of the molecular pathway of reprogramming had significantly progressed when specific transcription factors, such as Oct4, Sox2, Klf4, and c-Myc, were shown to collectively induce reprogramming of mouse fibroblasts into induced pluripotent stem cells (iPSCs; Takahashi and Yamanaka, 2006). Additional factors were reported to enhance reprogramming or to functionally substitute some of the mentioned factors (Maherali and Hochedlinger, 2008).
The core embryonic stem cell (ESC) regulatory circuitry includes Oct4, Sox2, and Nanog, which regulate their own expression and the expression of other factors involved in self-renewal and pluripotency (Hochedlinger et al., 2005). Although genetic experiments established that Oct4 and Sox2 are essential for pluripotency (Ivanova et al., 2006; Masui et al., 2007), the role of c-Myc and Klf4 in reprogramming is less clear.
Several reprogramming factors are known for their oncogenic activity, suggesting a tight link between stemness and cancer, and a possible involvement of reprogramming factors in the induction of cancer. Although c-Myc is a well known oncogene, Klf4 appears to posses both growth inhibitory and promoting capabilities, depending on the cell type (Evans and Liu, 2008). Oct4 can act as a dose-dependent oncogenic fate determinant, and its ectopic expression promotes dysplasia in epithelial tissues (Gidekel et al., 2003; Hochedlinger et al., 2005). In addition, up-regulation of Oct4, Sox2, and Nanog was reported in various tumors (Clark, 2007; Gu et al., 2007). Lin28, a factor required for reprogramming of human cells, also promotes transformation and plays a role in germ cell malignancies (Viswanathan et al., 2009; West et al., 2009). Furthermore, aggressive poorly differentiated human tumors were shown to express an ESC-like gene signature (Ben-Porath et al., 2008). These observations may derive from the role of stemness-inducing factors in maintaining high self-renewal and proliferative capacities, the hallmark of cancer cells.
In attempts to improve reprogramming efficiency, Zhao et al. (2008) demonstrated that the combination of p53 knockdown (KD) and Utf1 overexpression increases the efficiency of human iPSC generation (Zhao et al., 2008). The tumor suppressor p53, known as the guardian of the genome, is pivotal for cell cycle control and apoptosis (Levine and Oren, 2009) and was shown to control various differentiation programs of stem and progenitor cells (Molchadsky et al., 2008). Recent data demonstrate that p53 counteracts reprogramming via the well characterized p53 downstream pathways, namely induction of cell cycle arrest and apoptosis in DNA-damaged cells, ensuring the genomic integrity of the generated iPSC (Hong et al., 2009; Kawamura et al., 2009; Li et al., 2009; Marión et al., 2009; Utikal et al., 2009). In contrast, Hanna et al., (2009) claimed that p53 does not play a direct role in this process, and its effect is only a result of its function as a regulator of the proliferation rate of the cells. In other words, in p53-deficient cells the enhanced efficiency of reprogramming is in direct proportion to the increase in their proliferation rate.
p53 was also implicated in the core regulatory circuitry of ESCs. For example, p53 suppresses Nanog expression upon DNA damage in ESCs, resulting in their differentiation, thereby preventing them from proliferating in the presence of oncogenic stress (Lin et al., 2005). Moreover, activated p53 induces differentiation of human ESCs (Maimets et al., 2008). These studies are in agreement with the general notion that p53 is a growth-suppressor gene, and as such exerts its suppressing activity also in the reprogramming process. In that respect, p53 deficiency might exhibit a similar trait as overexpression of reprogramming factors, which may function both to promote reprogramming and, in the appropriate environment, exert an oncogenic activity. In other words, although inactivating p53 facilitates reprogramming, its reduced activity may also promote tumor development.
Mutations in p53 constitute a cornerstone in tumorigenesis. In this context, several p53 mutants were demonstrated to not only lose their WT function but also to acquire new properties, including the ability to interfere with the function of WT p53 and its family members, as well as additional p53-independent oncogenic functions. This notion is termed gain of function (GOF; Brosh and Rotter, 2009). Indeed, a long list of in vitro studies are now being confirmed by the conclusive data obtained from animal models (Lang et al., 2004; Olive et al., 2004; Terzian et al., 2008), showing that mutant p53 (mut-p53) germline animals are highly permissive to the development of aggressive cancers. A clue linking mut-p53 and reprogramming may reside in the finding that mut-p53 can interfere with cell differentiation (Matas et al., 2004; Shaulsky et al., 1991) and, thus, may promote the reverse process of dedifferentiation.
Our main goal was to study the role of mut-p53 in somatic cell reprogramming and to follow the in vivo fate of reprogrammed p53-deficient or mutated cells. To that end, we induced reprogramming of mouse embryonic fibroblasts (MEFs) that differ in their p53 status. WT, KD, KO, or mutant (mut-p53) knockin MEFs were reprogrammed by Oct4, Sox2, and Klf4 (three factors) or by only Oct4 and Sox2 (two factors). As previously reported (Hanna et al., 2009; Hong et al., 2009; Kawamura et al., 2009; Li et al., 2009; Marión et al., 2009; Utikal et al., 2009), we observed that p53 KD enhances the process of reprogramming. More importantly, however, we found that reprogramming of p53 KO MEFs with three factors led to the development of cells with a potential to form malignant tumors that occasionally displayed differentiated regions. In contrast, p53 KO cells reprogrammed with two factors maintained their pluripotent capacity also in vivo. Finally, mut-p53 exhibited a novel GOF activity by further enhancing reprogramming efficiency and reducing the differentiation capacity of MEFs reprogrammed by two factors in vivo. This novel GOF of mut-p53 is not attributed to its effect on proliferation rate, as both p53 KO and mut-p53 cells displayed a similar proliferation pattern, but the latter were much more prone for reprogramming and were more tumorigenic in vivo.
RESULTS
Enhanced reprogramming of MEFs expressing mut-p53 compared with p53 KO MEFs using Oct4, Sox2, and Klf4
In agreement with previous studies (Zhao et al., 2008; Hanna et al., 2009; Hong et al., 2009; Kawamura et al., 2009; Li et al., 2009; Marión et al., 2009; Utikal et al., 2009), we found that p53 counteracts the reprogramming process. By knocking down endogenous WT p53 in MEFs (p53 KD), we observed an enhanced reprogramming efficiency. Characterization of p53 KD iPSC clones demonstrated their ability to differentiate into typical cells of the three germ layers in vitro and in vivo, as evident by their ability to form teratomas and chimeric mice (Fig. S1). Thus, reprogramming of p53 KD cells resulted in the formation of bona fide iPSC.
Although p53 KD is quite efficient in MEFs, it does not completely eliminate p53 expression (Fig. S1 A and Fig. S2 B). Hence, we compared the effect of p53 KO to p53 KD on reprogramming efficiency. To this end, we infected control, p53 KD, and p53 KO MEFs with the three factors (Oct4, Sox2, and Klf4) together with GFP. Indeed, the fastest and highest reprogramming yield was achieved with p53 KO MEFs, followed by p53 KD MEFs and then by control infected MEFs (Fig. S2 A).
As demonstrated by others and in our experiments, p53 deficiency significantly increases the reprogramming rate of MEFs. However, it should be noted that loss of p53 function in human tumors is predominantly mediated by missense mutations, of which some were shown to possess novel properties. Therefore, it was of interest to examine whether mut-p53 plays a role along this process. To that end, we compared the reprogramming patterns of MEFs derived from p53 KO mice to those of MEFs derived from homozygous mut-p53 knockin mice, harboring an arginine-to-histidine substitution at aa 172 (Lang et al., 2004), corresponding to the R175H hotspot mutation in humans (p53R172H). These p53R172H MEFs, as well as p53 KO and WT p53 MEFs, were infected with retroviruses encoding Oct4, Sox2, Klf4, and GFP (p53R172H+3F, p53 KO+3F, and WT p53+3F). As demonstrated in Fig. 1 A, the colony number displaying alkaline phosphatase (AP) activity was significantly higher in p53R172H+3F MEFs compared with p53 KO+3F and WT p53+3F MEFs. Moreover, although 80% of isolated p53R172H+3F clones expressed Nanog already 4 wk after infection, none of the p53 KO+3F or WT p53+3F clones expressed Nanog at that time and started to accumulate it only 6 wk after the infection (Fig.1, A and B). It should be noted that reprogramming is a stochastic process, and quantifying the efficiency and timescales of this process has been problematic because of the cellular and genetic heterogeneity of de novo–infected somatic cells (Hanna et al., 2009; Yamanaka, 2009). Additionally, reprogrammed cells accumulate Nanog expression throughout the process. The kinetics of this accumulation is dependent upon the combined conditions of the specific reprogramming experiment (Jaenisch and Young, 2008). Therefore, it was important to use the same infection mixture for the compared cell types at the same time. The kinetic of reprogramming in our hands ranged between 4 and 6 wk. It is of note that because of the heterogeneity of each reprogramming process, and to validate our experiments, we conducted several experiments for each cell type with the different combinations of factors. These experiments were repeated under the same conditions using various batches of MEFs isolated from different mice. The pluripotency of both p53 KO+3F and p53R172H+3F clones was exhibited by their ability to undergo differentiation into cells of the three germ layers in vitro (Fig. 1 C). Overall, as summarized in Fig. 1, p53R172H MEFs were reprogrammed more efficiently than the other groups.
The efficiency of reprogramming with three factors is enhanced by p53R172H. (A, Left) WT p53, p53 KO, and p53R172H MEFs were infected with retroviruses encoding Oct4, Sox2, and Klf4 (three factors) and assayed for AP activity. Numbers indicate the mean amount of AP-positive colonies ± SE, obtained from duplicate plates. (A, Right) Clones with ES-like morphology were analyzed for Nanog expression by quantitative real-time PCR (QRT-PCR) at the indicated time points. The chart shows the percentage of Nanog-positive clones. Upon appearance of Nanog-positive clones in a certain MEF type, we maintained only these clones. Hence, measurement of Nanog-positive percentage is not applicable (N/A) for later time points. (B) Nanog mRNA relative expression, measured by QRT-PCR, 4 wk after infection in selected p53 KO and p53R172H iPS clones. ESCs served as a positive control. Results indicate the mean ± SD of two duplicate runs. A representative experiment out of three independent infections is shown for A and B. (C) In vitro differentiation of representative p53 KO+3F and p53R172H+3F clones (#107 and #m-11, respectively) into the three germ layers: mesoderm (smooth muscle, stained with smooth muscle actin [SMA] antibody), ectoderm (neurons, stained with β-III-tubulin antibody), and endoderm (hepatic cells, stained with α-fetoprotein [AFP] antibody). Bars, 50 µm. A representative experiment out of two is shown.
The efficiency of reprogramming with three factors is enhanced by p53R172H. (A, Left) WT p53, p53 KO, and p53R172H MEFs were infected with retroviruses encoding Oct4, Sox2, and Klf4 (three factors) and assayed for AP activity. Numbers indicate the mean amount of AP-positive colonies ± SE, obtained from duplicate plates. (A, Right) Clones with ES-like morphology were analyzed for Nanog expression by quantitative real-time PCR (QRT-PCR) at the indicated time points. The chart shows the percentage of Nanog-positive clones. Upon appearance of Nanog-positive clones in a certain MEF type, we maintained only these clones. Hence, measurement of Nanog-positive percentage is not applicable (N/A) for later time points. (B) Nanog mRNA relative expression, measured by QRT-PCR, 4 wk after infection in selected p53 KO and p53R172H iPS clones. ESCs served as a positive control. Results indicate the mean ± SD of two duplicate runs. A representative experiment out of three independent infections is shown for A and B. (C) In vitro differentiation of representative p53 KO+3F and p53R172H+3F clones (#107 and #m-11, respectively) into the three germ layers: mesoderm (smooth muscle, stained with smooth muscle actin [SMA] antibody), ectoderm (neurons, stained with β-III-tubulin antibody), and endoderm (hepatic cells, stained with α-fetoprotein [AFP] antibody). Bars, 50 µm. A representative experiment out of two is shown.
To exclude the possibility that the enhanced reprogramming of p53 KO or mutant MEF stems from increased infection yield, we measured GFP expression immediately after the infection. As shown in Fig. 2 A, the infection yield was similar in all three cell types (WT, KO, and mutant MEFs). It was recently suggested that the number of cell divisions is a key parameter controlling somatic cell reprogramming (Hanna et al., 2009). To determine whether p53 influences reprogramming via its affect on proliferation, we measured the proliferation rate of WT p53 MEFs compared with p53 KO MEFs. This revealed that despite the significantly higher reprogramming efficiency, the proliferation rate of p53-deficient MEFs was only three times higher than those of WT MEFs. Importantly, there was no growth advantage to mut-p53 MEFs over p53 KO MEFs (Fig. 2 B), although the former exhibit a dramatic increase in reprogramming efficiency. This clearly indicates that the reprogramming-promoting function of mut-p53 is not mediated via enhancement of proliferation, and it suggests that mut-p53 has a direct role in the reprogramming process.
Mut-p53 does not enhance MEF infection efficiency or possess a GOF activity in promoting MEF proliferation. (A) p53 KO, p53R172H, and WT MEFs were infected with three factors and GFP. The percentage of cells expressing GFP was measured 5 d after infection by flow cytometry. Noninfected MEFs were used as a negative control. A representative experiment out of two independent infections is shown. (B) Cumulative population doubling of uninfected WT p53, p53 KO, and p53R172H MEFs. A representative experiment out of two is shown.
Mut-p53 does not enhance MEF infection efficiency or possess a GOF activity in promoting MEF proliferation. (A) p53 KO, p53R172H, and WT MEFs were infected with three factors and GFP. The percentage of cells expressing GFP was measured 5 d after infection by flow cytometry. Noninfected MEFs were used as a negative control. A representative experiment out of two independent infections is shown. (B) Cumulative population doubling of uninfected WT p53, p53 KO, and p53R172H MEFs. A representative experiment out of two is shown.
In vivo growth of p53 KO and p53R172H clones reprogrammed by Oct4, Sox2, and Klf4
One of the hallmarks of iPSCs is their ability to form benign teratomas in Nude mice. A major concern using p53-deficient cells for reprogramming is their potential to undergo oncogenic transformation. Therefore, we focused on the in vivo fate of p53-deficient somatic cells that were reprogrammed into iPSC. Surprisingly, p53 KO+3F or p53R172H+3F MEFs, which exhibited pluripotent capacity in vitro, formed malignant tumors instead of teratomas. Specifically, injection of three representative p53 KO+3F clones (#w-103, 104, and 106) resulted in rapid growth of aggressive sarcomas (n = 6) with no apparent differentiated regions, whereas injection of two other p53 KO+3F clones (#110 and 103) resulted in formation of aggressive sarcomas (n = 4) with very limited differentiation capacity, giving rise to rare keratin foci (Fig. 3 A). Furthermore, injection of five p53R172H+3F clones resulted in rapid development of sarcomas (n = 5; clones #w-212, 213, and 204) or mixed tumors (n = 4; clones #m-7 and 11), consisting of malignant mesoderm with large regions of ectodermal differentiation, mostly into keratin (Fig. 3 B). This is in contrast to the benign teratomas we obtained by the injection of reprogrammed clones derived from WT, short hairpin (sh) control, and sh-p53–infected MEFs (Fig. S1). The cells were injected subcutaneously and the malignant tumors that resulted from this injection grew very rapidly (4–6 wk), necessitating euthanasia for ethical reasons. This time span is probably too short of the development of metastasis. However, we have thoroughly analyzed the invasive front of the various tumors summarized in Table S1. While all benign tumors did not show invasiveness, most of the malignant tumors grew in an infiltrative manner (Fig. S3). A full description of the tumors is summarized in Table S1. Combined, these in vitro and in vivo experiments suggest that complete p53 elimination or mutation not only enhances reprogramming induced by the three factors but also alters the nature of the reprogrammed cells, granting them cancer-forming potential.
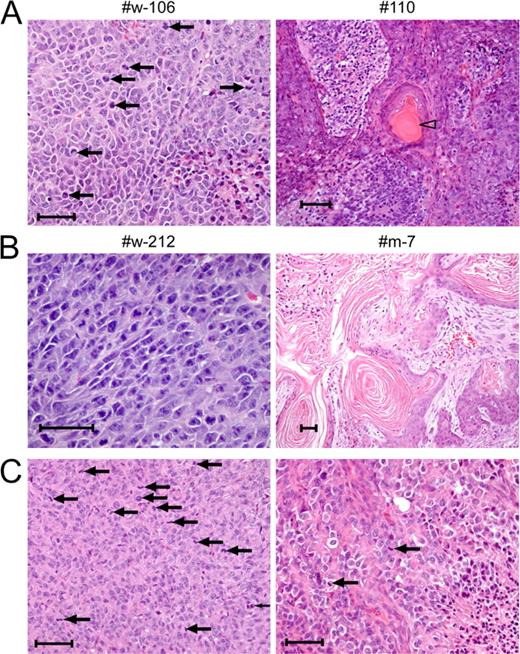
In vivo tumor formation by p53 KO+3F and p53R172H+3F clones and by Klf4-overexpressing p53 KO and p53R172H MEFs. (A, Left) A representative hematoxylin and eosin (H&E) section obtained from a typical sarcoma generated by a p53 KO+3F clone (#w-106). Arrows point at cells undergoing mitosis. (A, Right) A representative section of clone #110 that formed a sarcoma, within which were rare foci of keratin (arrowhead). Shown are representative sections out of 10 tumors that were analyzed. (B) Sarcoma (left) and a tumor containing large differentiated regions of keratin (right) generated by p53R172H+3F-reprogrammed clones (#w-212 and #m-7, respectively). Shown are representative sections out of nine tumors that were analyzed. (C) Typical sarcomas generated by Klf4-overexpressing p53 KO MEFs (left) and p53R172H MEFs (right). Arrows point at mitotic figures. Shown are representative sections out of two tumors analyzed for each cell type. The exact numbers of total tumors analyzed out of each representative clone are summarized in Table S1. Bars, 50 µm.
In vivo tumor formation by p53 KO+3F and p53R172H+3F clones and by Klf4-overexpressing p53 KO and p53R172H MEFs. (A, Left) A representative hematoxylin and eosin (H&E) section obtained from a typical sarcoma generated by a p53 KO+3F clone (#w-106). Arrows point at cells undergoing mitosis. (A, Right) A representative section of clone #110 that formed a sarcoma, within which were rare foci of keratin (arrowhead). Shown are representative sections out of 10 tumors that were analyzed. (B) Sarcoma (left) and a tumor containing large differentiated regions of keratin (right) generated by p53R172H+3F-reprogrammed clones (#w-212 and #m-7, respectively). Shown are representative sections out of nine tumors that were analyzed. (C) Typical sarcomas generated by Klf4-overexpressing p53 KO MEFs (left) and p53R172H MEFs (right). Arrows point at mitotic figures. Shown are representative sections out of two tumors analyzed for each cell type. The exact numbers of total tumors analyzed out of each representative clone are summarized in Table S1. Bars, 50 µm.
All reprogrammed clones were selected for isolation and further characterization according to their morphology. Interestingly, although the selected clones of both p53 KO and p53R172H showed typical iPSC morphology at lower passages, at later passages several clones changed their morphology and, instead of forming colonies with clear-cut round edges, spread and gave rise to amorphous-shaped colonies, which kept proliferating and took over the culture. Despite this dramatic change in morphology and growth control, the exogenous GFP was properly silenced in these clones. (Fig. S4). Importantly, malignant tumors developed from both early- and late-passaged clones and showed similar histological properties. However, tumor development was faster using late-passage clones (unpublished data).
The observation that p53 deficiency in MEFs diverts the reprogramming process toward malignant transformation led us to search for the underlying oncogenic driving force during the process of aberrant reprogramming. It was previously demonstrated that Klf4 could function as a tumor suppressor or an oncogene, depending on the cellular context (Evans and Liu, 2008). Therefore, we examined whether Klf4 expresses its oncogenic activity when introduced into p53-deficient MEFs. We infected either p53 KO or p53R172H MEFs with retroviruses encoding Klf4 and injected a pool of infected cells into Nude mice. This resulted in rapid formation of aggressive sarcomas (Fig. 3 C), whereas injection of noninfected p53 KO or p53R172H MEFs into Nude mice did not give rise to any tumors. These data indicate that Klf4 is capable of transforming p53 KO and p53R172H MEFs. Notably, WT p53 MEFs senesced either in the absence or presence of Klf4 overexpression and, thereby, could not have formed tumors in mice. In addition, overexpression of Klf4 in sh-p53 MEFs did not give rise to tumors up to 5 mo after infection. It should be noted that injection of only 100 cells from selected reprogrammed clones, or from p53 KO/p53R172H MEFs overexpressing Klf4, resulted in tumor formation as well (Table I). Furthermore, we have generated several cell lines derived from selected tumors and injected these cells into Nude mice to determine the potential of these tumor-derived cell lines to give rise to secondary tumors. As shown in Table I, we obtained secondary tumors from p53R172H+3F clones. These tumors maintained the characteristics of their parental tumors, i.e., either a sarcoma (#w-212) or a tumor with regions of ectodermal differentiation, mostly into keratin, and malignant mesoderm (#m-11; unpublished data). It is of note that the injection of only 10 cells of p53 KO+Klf4 tumor–derived cells was sufficient to induce tumor formation, indicating the high tumorigenic potential of these cells. Combined, these results clearly show that in p53-deficient primary MEFs, Klf4 can exert its oncogenic potential and that the malignant phenotype of reprogrammed cells generated by the three factors in a p53-deficient environment may be attributed to the oncogenic activity mediated by Klf4.
Tumor forming potency of the divergent cell types
| Cell type | 100 cells | 1,000 cells | 10,000 cells |
| p53R172H+3F (#m-11) | 1/4 | 1/4 | 4/4 |
| p53R172H+3F (#w-212) | 3/4 | 4/4 | N/A |
| p53R172H+2F (#T-15) | 1/2 | 2/2 | 1/2 |
| p53 KO+2F (#226) | 0/4 | 2/2 | 1/2 |
| p53 KO+3F (# 103) | 3/4 | 3/4 | 2/4 |
| sh-con+3F (#I) | 1/2 | 0/2 | 0/2 |
| p53 KO Klf4 | 4/4 | 4/4 | N/A |
| p53R172H Klf4 | 1/2 | 1/2 | N/A |
| sh-p53+ Klf4 | 0/4 | 0/2 | 0/2 |
| Tumor-derived #m-11 | 1/2 | N/A | N/A |
| Tumor-derived #w-212 | 1/2 | N/A | N/A |
| Tumor-derived p53 KO Klf4 | 1/2 (also 1/2 after injection of only 10 cells) | N/A | N/A |
| Cell type | 100 cells | 1,000 cells | 10,000 cells |
| p53R172H+3F (#m-11) | 1/4 | 1/4 | 4/4 |
| p53R172H+3F (#w-212) | 3/4 | 4/4 | N/A |
| p53R172H+2F (#T-15) | 1/2 | 2/2 | 1/2 |
| p53 KO+2F (#226) | 0/4 | 2/2 | 1/2 |
| p53 KO+3F (# 103) | 3/4 | 3/4 | 2/4 |
| sh-con+3F (#I) | 1/2 | 0/2 | 0/2 |
| p53 KO Klf4 | 4/4 | 4/4 | N/A |
| p53R172H Klf4 | 1/2 | 1/2 | N/A |
| sh-p53+ Klf4 | 0/4 | 0/2 | 0/2 |
| Tumor-derived #m-11 | 1/2 | N/A | N/A |
| Tumor-derived #w-212 | 1/2 | N/A | N/A |
| Tumor-derived p53 KO Klf4 | 1/2 (also 1/2 after injection of only 10 cells) | N/A | N/A |
The potency of the designated cell types to form tumors was analyzed by subcutaneous injection of various amounts of the designated cells (100, 1,000, or 10,000 cells) into Nude mice. Indicated are the numbers of animals out of total animals analyzed in which a tumor developed within 4 mo. For some cell types, only low numbers of cells were injected; therefore, estimation of tumor formation following injection of high numbers of cells was not applicable (N/A).
One of the hallmarks of p53 is to maintain chromosomal integrity and stability. To further characterize the effect of p53 deficiency on the genomic stability of reprogrammed cells, we used spectral karyotyping analysis of representative clones used throughout our studies. As expected, the karyotype of WT MEFs, even at low passages, is very unstable, comprising several chromosomal duplicates in most of the cells (Table S2). This chromosomal instability of normal primary cultures of mesenchymal stem/progenitor cells is well known and does indicate the cells’ tumorigenic potential (Tolar et al., 2007; Foudah et al., 2009; Holland and Cleveland, 2009; Josse et al., 2010). To gain tumorigenic potential, the cells must acquire additional mutations in specific oncogenes/tumor suppressors. Indeed, as mentioned before, injection of p53 KO and mutant MEFs, which display similar levels of chromosomal instability, did not result in tumor formation.
The karyotype picture was identical in p53 KO and mutant MEFs, yielding the same abnormal chromosomal number as WT-MEFs. Interestingly, however, although reprogrammed cells originating from p53 KO and mutant MEFs retained this chromosomal abnormality, reprogrammed cells originating from either WT MEFs, or even from p53 KD MEFs, exhibited a rather normal chromosomal picture, albeit with some minor insertions (Table S2), suggesting that the presence of p53 is essential for maintaining the genomic integrity of reprogrammed cells.
A novel GOF of mut-p53 in reprogramming cells using only Oct4 and Sox2
As p53 was shown to be a negative regulator of Nanog (Lin et al., 2005; Rowland et al., 2005) and Klf4 was shown to suppress p53 expression, it was previously hypothesized that Klf4 may contribute to reprogramming by its p53-suppressive activity. Providing that this assumption is correct, Klf4 should be dispensable for reprogramming of p53 KO MEFs. Although p53-deficient fibroblasts were reprogrammed with only Oct4 and Sox2, albeit with lower efficiency (Kawamura et al., 2009), another group reported that Klf4 is essential for reprogramming p53-deficient fibroblasts (Zhao et al., 2008). Because of the oncogenic activity of Klf4, which was manifested in p53-deficient cells, we examined whether reprogramming of p53-deficient MEFs with only Oct4 and Sox2 will result in the formation of normal iPSC. In agreement with Zhao et al. (2008), we found that Klf4 is essential for reprogramming of p53 KO MEFs because 2 mo after infection there was only a slight increase in expression of stemness markers in isolated clones (unpublished data). However, prolonged culturing of these clones (for 5 mo) resulted in the establishment of four clones that exhibited iPSC characteristics, including expression of stemness markers (Fig. 4 A). The pluripotency of these clones was evident by their ability to differentiate into cells of the three germ layers in vitro and to form teratomas in vivo (Fig. 4, B and C, respectively). Surprisingly, a careful examination of the histopathology of the teratomas revealed that five out of seven tumors derived from these clones (#202–6, 202, 203, and 226) contained various levels of malignant mesenchyme characteristic of teratocarcinoma instead of benign teratoma (Fig. 4 D). Moreover, one of the injected clones (#226) that gave rise to a teratocarcinoma also gave rise to a tumor comprising both sarcoma and carcinoma cells, with no detectable differentiated regions (Fig. 4 D). These data suggest that the p53 KO clones that were reprogrammed with only Oct4 and Sox2 (excluding Klf4) represent a population of pluripotent cells with the capacity to initiate the formation of both benign and malignant tumors. It should be noted that no clones were formed when WT-p53 or sh-p53 MEFs were used under the same experimental conditions (unpublished data).
Reprogramming of p53 KO MEFs with Oct4 and Sox2. (A) Relative expression of mRNA encoding endogenous stemness markers Fbxo15, Sox2, and Oct4 was measured by QRT-PCR 5 mo after infection of MEFs with retroviruses encoding Sox2 and Oct4. iPS clones that appeared 5 mo after infection are indicated. Uninfected MEFs are used as negative controls and ESCs as a positive control. The results are represented by the mean ± SD of two duplicate runs from a representative experiment out of two individual infections. (B) In vitro differentiation into cells of the three germ layers of a representative p53 KO+2F clone (#202-3). Markers used are described in Fig. 1 C. Bars, 100 µm. Shown is a representative experiment out of two. (C) Representative H&E sections of a teratoma formed from a p53 KO+2F clone (#202-3) with representation of the three germ layers. (D, Left) irregular islands of epithelial differentiation showing marked dysplasia and high mitotic rate (arrowheads) in a tumor generated by the p53 KO+2F clone #226. In the center of the field there is a band of plump spindle cells (mesoderm), including one mitotic figure (arrow). Shown is a representative of five tumors showing various levels of malignancy. (D, Right) The inset magnification depicts a group of malignant epithelial cells (carcinoma). To their left are malignant spindle cells of mesodermal origin (sarcoma). Arrows indicate mitotic figures. Bars, 50 µm.
Reprogramming of p53 KO MEFs with Oct4 and Sox2. (A) Relative expression of mRNA encoding endogenous stemness markers Fbxo15, Sox2, and Oct4 was measured by QRT-PCR 5 mo after infection of MEFs with retroviruses encoding Sox2 and Oct4. iPS clones that appeared 5 mo after infection are indicated. Uninfected MEFs are used as negative controls and ESCs as a positive control. The results are represented by the mean ± SD of two duplicate runs from a representative experiment out of two individual infections. (B) In vitro differentiation into cells of the three germ layers of a representative p53 KO+2F clone (#202-3). Markers used are described in Fig. 1 C. Bars, 100 µm. Shown is a representative experiment out of two. (C) Representative H&E sections of a teratoma formed from a p53 KO+2F clone (#202-3) with representation of the three germ layers. (D, Left) irregular islands of epithelial differentiation showing marked dysplasia and high mitotic rate (arrowheads) in a tumor generated by the p53 KO+2F clone #226. In the center of the field there is a band of plump spindle cells (mesoderm), including one mitotic figure (arrow). Shown is a representative of five tumors showing various levels of malignancy. (D, Right) The inset magnification depicts a group of malignant epithelial cells (carcinoma). To their left are malignant spindle cells of mesodermal origin (sarcoma). Arrows indicate mitotic figures. Bars, 50 µm.
Because reprogramming of p53 KO cells with only two factors is an extremely inefficient process, we wondered whether mut-p53 will enhance its efficiency, similar to its enhancing the capacity of reprogramming by three factors. Indeed, the total number of clones with typical iPSC characteristics was significantly enhanced in p53R172H MEFs compared with p53 KO and WT p53 MEFs reprogrammed with Oct4 and Sox2 (p53R172+2F, p53 KO+2F, and WT p53+2F; Fig. 5 A). Moreover, 16 of the 19 (84%) isolated p53R172H+2F clones expressed high levels of Nanog already 50 d after the infection, whereas none of the 12 selected p53 KO+2F clones expressed Nanog at the same time point (Fig. 5 B). In addition to Nanog, all selected p53R172H+2F clones expressed high levels of endogenous Oct4 and Sox2, whereas only some of the selected p53 KO+2F clones expressed these genes at the same time and to a lower extent (Fig. 5 B). The morphology of p53R172H+2F clones and p53 KO+2F clones was typical to that of normal iPSC. However, although in most of the p53R172H+2F clones the exogenous GFP was silenced 24 d after the infection, p53 KO+2F clones still expressed GFP at that stage (Fig. S5), and silencing occurred only at a later culturing period (not depicted). These results suggest a novel GOF property for mut-p53 in the process of reprogramming.
GOF of mut-p53 in enhancing the reprogramming efficiency of MEFs using only Oct4 and Sox2. (A) Comparison of reprogramming efficiency of WT p53 (WT), p53 KO, and p53R172H MEFs by retroviruses encoding Oct4 and Sox2. After infection, clones with typical iPSC characteristics in vitro were counted at the indicated time points. (B) Comparison of Nanog (top) and endogenous Sox2 and Oct4 mRNA (bottom) expression between selected p53 KO+2F and p53R172H+2F clones, measured by QRT-PCR 50 d after infection. A representative experiment out of three individual infections is shown for A and B. (C) Basal expression levels of mRNA encoding stemness markers Nanog, Sox2, and Oct4 in WT p53, p53 KO, and p53R172H MEFs. A representative experiment out of at least five independent analyses of MEFs derived from various preparations is shown. Results indicate the mean ± SD of two duplicate runs.
GOF of mut-p53 in enhancing the reprogramming efficiency of MEFs using only Oct4 and Sox2. (A) Comparison of reprogramming efficiency of WT p53 (WT), p53 KO, and p53R172H MEFs by retroviruses encoding Oct4 and Sox2. After infection, clones with typical iPSC characteristics in vitro were counted at the indicated time points. (B) Comparison of Nanog (top) and endogenous Sox2 and Oct4 mRNA (bottom) expression between selected p53 KO+2F and p53R172H+2F clones, measured by QRT-PCR 50 d after infection. A representative experiment out of three individual infections is shown for A and B. (C) Basal expression levels of mRNA encoding stemness markers Nanog, Sox2, and Oct4 in WT p53, p53 KO, and p53R172H MEFs. A representative experiment out of at least five independent analyses of MEFs derived from various preparations is shown. Results indicate the mean ± SD of two duplicate runs.
As described, Klf4 was suggested to contribute to reprogramming by the suppression of p53. However, the reprogramming efficiency of p53-deficient fibroblasts with only two factors was much lower compared with WT-p53 fibroblasts reprogrammed with three factors. As p53 KO did not substitute for Klf4, it is clear that, besides p53 suppression, Klf4 promotes reprogramming by additional mechanisms. In contrast, in the presence of p53R172H, the efficiency of reprogramming with only two factors was even higher than WT-p53 MEFs reprogrammed by three factors. Thus, p53R172H exhibits an additional GOF activity by compensating for the lack of Klf4 in efficient reprogramming and may be considered as a reprogramming factor.
In an attempt to unveil the mechanism underlying the newly dependent unidentified activity of p53R172H in reprogramming, we measured the basal levels of stemness factors in p53R172H MEFs. Interestingly, these MEFs expressed higher basal levels of Nanog, Sox2, and Oct4 than p53 KO and WT p53 MEFs (Fig. 5 C). Immunostainings of WT p53, p53 KO, p53R172H MEFs, and ESC, using antibodies against Oct4, Sox2, and Nanog, detected the expression of endogenous Oct4, Sox2, and Nanog in ESCs but failed to detect any endogenous expression by p53R172H MEFs (unpublished data). This suggests that the higher basal levels observed by RT-PCR may reflect a moderate increase in the expression of these genes in the entire population rather than pronounced increase in few cells. Because the expression of these genes by p53R172H MEFs is much lower than the levels expressed by ESCs (∼1/10), their encoded proteins probably cannot be detected by the commercial antibodies used. As demonstrated for adult neural stem cells (Kim et al., 2009), the increased basal expression levels of these stemness factors in p53R172H MEFs might render them more prone to reprogramming.
Finally, selected p53R172H+2F clones were further characterized for their pluripotent capacity. As demonstrated in Fig. 6 A, they were able to differentiate into cells of the three germ layers in vitro. However, injection of these clones into Nude mice resulted in the development of tumors similar to those obtained from p53R172H clones reprogrammed with three factors, i.e., tumors with limited differentiation capacity, mainly to keratin and epithelial tissues, surrounded by highly malignant mesenchyme and invasive front (n = 6; clones #t-15, t-20, and t-4; Fig. 6 B and Fig. S3). In addition, one clone (#t-8) gave rise to sarcomic tumors (n = 2) with no differentiation (Fig. 6 B). Thus, in addition to the GOF activity of p53R172H in enhancing the efficiency of the process, p53R172H+2F clones differ from p53 KO+2F in their characteristics. Although p53 KO+2F clones still maintain their pluripotential capacity in vivo, p53R172H+2F clones exhibit very limited differentiation capacity.
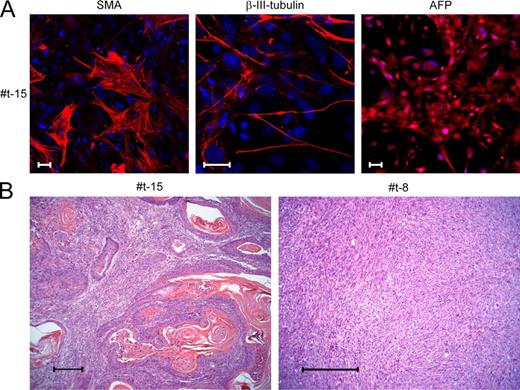
p53R172H cells reprogrammed with Oct4 and Sox2 lose their differentiation capacity in vivo. (A) In vitro differentiation into cells of the three germ layers of a representative p53R172H+2F clone (#t-15). Markers used are described in Fig.1 C. Bars, 25 µm. A representative experiment out of two is shown. (B) Representative sections obtained from tumors formed by p53R172H+2F clones. Left, a sarcoma containing large regions of ectodermal differentiation (#t-15). Right, a sarcoma without any differentiation (#t-8). Bars, 100 µm. Shown are representative sections out of eight tumors that were analyzed. The exact numbers of total tumors analyzed out of each representative clone are summarized in Table S1.
p53R172H cells reprogrammed with Oct4 and Sox2 lose their differentiation capacity in vivo. (A) In vitro differentiation into cells of the three germ layers of a representative p53R172H+2F clone (#t-15). Markers used are described in Fig.1 C. Bars, 25 µm. A representative experiment out of two is shown. (B) Representative sections obtained from tumors formed by p53R172H+2F clones. Left, a sarcoma containing large regions of ectodermal differentiation (#t-15). Right, a sarcoma without any differentiation (#t-8). Bars, 100 µm. Shown are representative sections out of eight tumors that were analyzed. The exact numbers of total tumors analyzed out of each representative clone are summarized in Table S1.
Activation of mut-p53 in tumors formed by reprogrammed p53R172H MEFs
Accumulation of the p53 protein in mut-p53 knockin mice was demonstrated to occur only in tumors and transformed cells and not in normal tissues (Lang et al., 2004; Terzian et al., 2008; Wang et al., 2009). Moreover, ample data indicate that stabilization and accumulation of mut-p53 enhances its dominant-negative and GOF abilities (Brosh and Rotter, 2009). Therefore, we wondered whether mut-p53 protein level is altered during the processes of in vitro reprogramming and in vivo tumor formation. We found that p53R172H-reprogrammed clones exhibited similar mut-p53 protein levels to their parental p53R172H MEFs (Fig. 7 A). However, comparison of three pairs of p53R172H-reprogrammed clones to the tumors derived from these clones revealed that mut-p53 is stabilized in those tumors (Fig. 7 B). Specifically, although the clones growing in vitro express a single form of p53 of comparable size and level to that found in their parental p53R172H MEFs, their corresponding tumors accumulate several p53 forms, which may represent activated mut-p53 (Brosh and Rotter, 2009). This may explain the discrepancy between in vitro and in vivo results. Although in vitro mut-p53 is not accumulated and, thereby, does not abrogate proper differentiation of the reprogrammed cells, its accumulation in vivo probably results in its enhanced activation, which may lead to perturbation of differentiation, eventually resulting in formation of malignant tumors. Analyses of the pattern of mut-p53 expression in the tumors revealed that it is expressed only by part of the tumor cells (Fig. 7 C), suggesting that its expression/activation is regulated within the tumor and associated with selected tumor cell populations. It is of note that in some tumors its expression was excluded from differentiated regions (Fig. 7 C, top).
p53R172H-reprogrammed cells form tumors that accumulate mut-p53 in restricted regions. (A) A Western blot depicting the level of mut-p53 in p53R172H MEFs and selected p53R172H-reprogrammed clones (reprogrammed by two or three factors, as indicated). (B) A Western blot depicting mut-p53 accumulation in tumors derived from p53R172H clones (reprogrammed by two or three factors, as indicated). (C) Representative tumor sections derived from p53R172H-reprogrammed clones were stained with anti-p53 (brown). The stained sections were counterstained with hematoxylin (blue). Top, the most well differentiated cells, arranged as a band (asterisks), possibly tumor stroma, do not express p53. Bar, 200 µm. Bottom, intensive positive staining for mut-p53 is present in some but not all neoplastic cells. Arrows indicate differentiated regions of keratin foci. Bar, 400 µm. Stainings were performed using five different tumors.
p53R172H-reprogrammed cells form tumors that accumulate mut-p53 in restricted regions. (A) A Western blot depicting the level of mut-p53 in p53R172H MEFs and selected p53R172H-reprogrammed clones (reprogrammed by two or three factors, as indicated). (B) A Western blot depicting mut-p53 accumulation in tumors derived from p53R172H clones (reprogrammed by two or three factors, as indicated). (C) Representative tumor sections derived from p53R172H-reprogrammed clones were stained with anti-p53 (brown). The stained sections were counterstained with hematoxylin (blue). Top, the most well differentiated cells, arranged as a band (asterisks), possibly tumor stroma, do not express p53. Bar, 200 µm. Bottom, intensive positive staining for mut-p53 is present in some but not all neoplastic cells. Arrows indicate differentiated regions of keratin foci. Bar, 400 µm. Stainings were performed using five different tumors.
DISCUSSION
In this study, we reprogrammed a series of MEFs differing in their p53 status, which greatly influenced both the efficiency of reprogramming and the nature of the reprogrammed cells (Fig. S6 and Table S1). The tumor suppressor p53, which plays a pivotal role in maintaining genome fidelity (Levine and Oren, 2009), was recently demonstrated to counteract somatic cell reprogramming (Zhao et al., 2008; Hong et al., 2009; Kawamura et al., 2009; Li et al., 2009; Marión et al., 2009; Utikal et al., 2009). Specifically, inhibiting p53 activity, using strategies such as KD, KO, or overexpression of dominant-negative forms, increased reprogramming efficiency of a variety of mouse and human somatic cells. However, considering the role of p53 as a genome caretaker, its deficiency may lead not only to the acceleration of reprogramming but also to oncogenic transformation of the iPSCs generated, diminishing their therapeutic potential. Because p53 is mostly mutated in tumors and mut-p53 was shown to possess novel activities, our major goal was to study the role of mut-p53 in this process and to follow the in vivo fate of reprogrammed p53-deficient somatic cells. In agreement with the aforementioned studies, we found that reduction in p53 levels accelerated typical reprogramming of MEFs. In our initial experiments we reprogrammed MEFs using the three factors: Oct4, Sox2, and Klf4. This resulted in a gradual p53-dependent increase in the reprogramming efficiency of MEFs as follows: WT-p53 < sh-p53 < p53 KO < p53R172H. This pattern was even more pronounced when only two factors, Oct4 and Sox2, were used. Although under in vitro conditions no major differences in the general characteristics of these clones were noticed, their injection into mice revealed differences in the nature of these cells. In contrast to WT-p53 and sh-p53 cells, the complete p53 elimination or the expression of its mutated form resulted in reprogrammed cells that, along with their pluripotential capacity, embodied tumorigenic potential. These typical reprogrammed single-cell clones, when injected into mice formed tumors that exhibited a mixed phenotype, comprising both differentiated regions and highly malignant cells. Overall, the increase in reprogramming efficiency correlates with the capacity of these clones to form aggressive tumors.
Mut-p53 exhibits a novel GOF by enhancing the efficiency of reprogramming with three factors, and a more prominent GOF emerges by using only 2Fs. Although the generation of p53 KO+2F clones is a very inefficient process, the presence of mut-p53 compensated for the lack of Klf4, yielding high numbers of reprogrammed clones in a relatively short period. This novel activity of mut-p53 was accompanied not only by affecting the process quantitatively but also by changing the qualitative features of the reprogrammed cells. Although p53 KO+2F clones maintained their pluripotential capacity in vivo, and gave rise to teratomas and teratocarcinomas, p53R172H+2F clones lost their differentiation capacity in vivo, giving rise mainly to sarcomas.
As for the reported duality of Klf4, which, depending on the cellular circumstances, may function either as a tumor suppressor or an oncogene (Evans and Liu, 2008), in our study Klf4 functions as an oncogene, as its overexpression alone in either p53 KO or p53R172H MEFs induced aggressive tumors. Moreover, even in the presence of its reprogramming partners (Oct4 and Sox2), Klf4 seems to possess oncogenic potential, as p53 KO+2F clones could form well differentiated tumors, whereas p53 KO+3F clones formed only poorly differentiated sarcomas. It should be noted that although the exogenous genes are silenced during the process, the silencing takes place only after cells are already reprogrammed and start to express DNA methyltransferases (Takahashi and Yamanaka, 2006). Thereby, expression of oncogenes in this process, even at early stages, may contribute to the formation of malignant cells. Additionally, this is in accordance with previous data demonstrating the high oncogenic activity of c-Myc, which was shown to accelerate reprogramming, yielding iPSC, which gave rise to mice with high incidence of cancer caused by reactivation of the c-Myc transgene (Okita et al., 2007). Thus, reactivation of the Klf4 transgene may contribute to tumor formation in vivo. Accordingly, we analyzed whether Oct4 and Sox2 possess oncogenic activity as well. For that, p53 KO and mut-p53 cells were infected with either Oct4 or Sox2, and the pool of infected cells was injected to Nude mice. Although injections with Sox2-infected cells did not give rise to tumors, a small part of mice injected with Oct4-infected cells developed tumors (unpublished data). This may explain the tumorigenic potential of p53 KO+2F. However, although most p53 KO+2F clones gave rise to teratomas or teratocarcinomas, p53R172H+2F clones gave rise mostly to sarcomas, suggesting that mut-p53 gains a novel activity and functions as an oncogene in this process. Mut-p53 was previously shown to hold a differentiation-blocking activity and to affect proper cellular maturation as well (Shaulsky et al., 1991; Matas et al., 2004; Wang et al., 2009). Our results demonstrate the expression of mut-p53 in undifferentiated regions of the tumors (Fig. 7 C). Given that maturational arrest is suggested as a possible mechanism of cancer formation (Sell, 2004), the oncogenic activity of mut-p53 in reprogramming may be attributed to its abrogation of differentiation function.
Our results are in agreement with the notion that differentiation and malignant transformation may represent reciprocal situations. Reprogramming of somatic cells into ES-like cells requires precise orchestration between dedifferentiation, immortalization, and the acquisition of pluripotency and self-renewal properties. Perturbation in the balance between these processes could lead to the acquisition of aberrant properties. The low efficiency of reprogramming may stem from the fact that during this multistep process, analogous to tumorigenesis (Hanahan and Weinberg, 2000), a cell lineage should stochastically accumulate several genetic and epigenetic alterations. Indeed, there is a tight link between pluripotency and tumorigenesis (Knoepfler, 2009). Reprogramming of cells malfunctioned in their tumor-suppressing machinery may raise the probability of oncogenic transformation. One of the main functions of p53 is to maintain chromosomal integrity and stability, which was previously shown to also occur in ESCs (Lin et al., 2005). In addition, Marión et al. (2009) demonstrated the requirement of p53 to ensure the genomic integrity of iPSC. p53-null iPSC showed chromosomal instability and persistent damaged DNA, which was also demonstrated in teratomas derived from these cells. This suggests the possible malignancy of these tumors, although it was not further characterized. The karyotype analysis of the various reprogrammed cells generated in our study revealed that although reprogrammed cells originating from p53 KO and mutant MEFs retained the chromosomal abnormality of the parental MEFs, reprogrammed cells originating from WT MEFs, or even from p53 KD MEFs, exhibited a rather normal chromosomal picture (Table S2). This suggests that, indeed, the presence of p53 is essential for reprogramming of selected cells with normal chromosomal numbers (or harboring minor changes). Alternatively, it may also suggest that in the presence of WT p53, reprogrammed cells carrying gross chromosomal aberrations are eliminated from the population by either programmed cell death or growth arrest.
Our data show that a pluripotential capacity in vivo does not guarantee the fidelity of iPSC because reprogrammed clones that gave rise to teratomas held a potential to also form malignant tumors. These data suggest that the various clones generated actually represent mixtures of stem cells and cancer-forming cells at different ratios. It is therefore important to note that as long as there are no reliable markers to distinguish between normal stem cells and cancer-forming cells, it is difficult to asses the actual balance between stemness and cancer that will be expressed in vivo. Indeed, there is an increasing body of evidence supporting the notion that tumors are populated by fractions of cells with stem cell–like properties (Reya et al., 2001; Kim and Dirks, 2008). This has been shown for certain leukemias (Lapidot et al., 1994) and breast (Al-Hajj et al., 2003) and brain (Amariglio et al., 2009) tumors. Furthermore, it was also shown that leukemic stem cells express antigens similar to those expressed by hematopoietic stem cells (Taussig et al., 2005). It was also suggested that most tumors arise from the maturational arrest of a cellular lineage derived from a tissue stem cell (Sell, 2004), providing links between stem cells, tumor-initiating cells, and cancer formation. Accordingly, we observed that reprogramming of MEFs may give rise to cells which display characteristics of either stem cells or cancer cells at various ratios, depending on p53 status. As somatic cells are continuously exposed to external and internal genotoxic stress, the relatively low incidence of tumor development is puzzling unless we assume that there is another significant barrier on the path to cancer. Based on our findings, we speculate that a productive malignant transformation is also dependent on the genomic elasticity of cells. Stem cells, having unstable genomes, provide such a suitable cellular environment for a productive transformation. In fact, to permit the pluripotency of stem cells, genomic elasticity is required (Hochedlinger and Plath, 2009). It is therefore possible that under such flexible genomic conditions, loss of genomic stability, such as that mediated by p53 loss or mutation, may be abused by oncogenes to override normal cellular fate and, instead, embark on the chaotic road toward malignant transformation. This may underlie the high incidence of cancer development in Li-Fraumeni syndrome patients, who usually bear germline mutations in p53 (Malkin et al., 1990; Srivastava et al., 1990).
Recently, the six essential features characteristic of cancer cells, suggested by Hanahan and Weinberg (2000), were revisited (Lazebnik, 2010). The major difference between cancerous and benign tumors is the tissue invasion and metastatic features of the former. ESCs and iPSCs can form benign tumors. However, the presence of mut-p53 tips the scale toward the formation of malignant tumors, or, in other words, toward cancer formation. Establishing these divergent clones, with the capacity to induce either benign or malignant tumors with various differentiation capacities, may serve as a platform to answer the challenging question of the mechanism underlying the key emergent property of cancers: their malignancy.
In sum, our present study shows that p53 plays both a quantitative role, determining the efficiency of reprogramming, and a qualitative regulatory role, determining the fidelity of the reprogrammed cells. Accelerating the process, without proper checkpoints enabling DNA damage repair or cell death of impaired cells, leads to the formation of reprogrammed cells that, besides acquiring the pluripotential feature, hold unstable DNA and the potential to initiate cancer formation. In contrast to the differentiation-promoting in vitro conditions, this trait is revealed only in vivo, where the appropriate microenvironment enables small numbers of such mutated cells, in which differentiation is abrogated, to take over most of the tumor cell population. The presence of mut-p53 further promotes reprogramming efficiency along with tumorigenicity of the reprogrammed cells.
MATERIALS AND METHODS
Cell culture.
Primary MEFs were prepared from 13.5 d postcoitum embryos. MEFs were maintained in DME, supplemented with 10% FCS and antibiotics. Phoenix retrovirus-producing cells were obtained from the American Type Culture Collection. The R1-ESC line and iPSCs were cultured in DME supplemented with 15% FCS, 1 mM sodium pyruvate, 2 mM L-Glutamine, 0.1 mM nonessential amino acids, 0.1 mM β-mercaptoethanol, 1,000 U/ml LIF (ESG1107 [Millipore] and rhuman LIF [bioLEAD]), and pen/strep (ES medium). For induction of in vitro differentiation, 106 cells were plated in bacterial plates with DME supplemented with 10% horse serum and 4 U/100 ml insulin (Humulin; Lilly Diabetes) for 5–9 d. The embryoid bodies formed were plated on gelatin-coated coverslips for 14–20 d using the same medium.
Retroviral constructs, infections, and iPSC generation.
For p53 KD, mouse-specific p53 sh-RNA (sh-p53) vector and human-specific Rb-shRNA control (sh-con) vector were used (provided by S. Lowe, Cold Spring Harbor Laboratory, Cold Spring Harbor, NY). Cells were selected with Puromycin for 1 wk before the infection with the reprogramming factors. Sox2, Oct4, and Klf4 expression vectors (Takahashi and Yamanaka, 2006) were purchased from Addgene. pWZL-GFP-blasticidin vector was provided by W. Hahn (Dana-Farber Cancer Institute, Boston, MA). Retroviral infection procedures were performed using Phoenix cells, as previously described (Kochupurakkal et al., 2008). 1 d after infection, 3.5 × 105 cells were plated on irradiated feeder MEFs in ES medium. The cells were later transferred to gelatin-coated plates. When colonies emerged (4–6 wk after infection), they were isolated and passaged separately.
Immunocytochemistry.
Immunocytochemistry was performed as previously described (Sarig et al., 2006) with primary antibodies against smooth muscle actin (1:500; A2547; Sigma-Aldrich), 1 drop of α1-fetoprotein (N150130; Dako), or TUJ1 (1:400; ab14545; Abcam), and with appropriate secondary antibodies (Jackson ImmunoResearch Laboratories). DAPI staining was used to visualize nuclei.
AP activity.
AP activity was performed as previously described (Kochupurakkal et al., 2008). Colonies number was determined using Image-Pro software (Media Cybernetics).
Reverse transcription and RT-PCR.
QRT-PCR was performed as previously described (Molchadsky et al., 2008). Reactions were performed in duplicates and error bars in charts represent SD. Semi-Q-PCR was performed using ready mix (Bio-Lab Ltd.). Oct4-, Sox2-, and Klf4-specific primers were designed for either total or endogenous mRNA. Table S3 lists primer sequences.
Western blot analysis.
Western blotting was performed as previously described (Molchadsky et al., 2008) with the following antibodies: rabbit anti–mouse p53 (produced in our laboratory) and anti–mouse p53 monoclonal pAb240 (Yewdell et al., 1986).
Tumor formation and analysis.
ESCs or selected reprogrammed clones were trypsinized and replated with ES medium for 15 min. Nonadherent cells were collected, resuspended in PBS, and injected subcutaneously into Nude mice (106 cells/100 µl, with Matrigel matrix [BD] at a ratio of 1:1). The tumors were removed 2–16 wk after injection, fixed in 4% paraformaldehyde, decalcified, and embedded in paraffin blocks. Sections, taken from three levels, were stained with H&E. The designation of a tumor as benign or malignant was based on histological criteria. It took into account the cytological features of nondifferentiated stromal tissue composed of spindle-shaped cells. Tumors considered malignant were typically densely cellular, composed of pleomorphic cells with a high nuclear/cytoplasmic ratio, showed anisocytosis and anisokaryosis, and had a high mitotic rate. Many, but not all, showed an infiltrative growth pattern. In contrast, the stroma in benign tumors was typically well differentiated and of low to intermediate cellularity. Its growth pattern was expansile, pushing rather than infiltrating surrounding tissues. Slightly malignant is admittedly an imprecise designation, indicating that the tumor showed features intermediate between these two extremes.
Where indicated, cells collected from selected reprogrammed clones were diluted before injections (104/103/102/101 cells/50 µl, with Matrigel matrix at a ratio of 1:1). The tumors were removed 6–16 wk after injection and subjected to histology analyses as in the previous paragraph. Tumor-derived cell lines were generated out of part of the tumors by dissociating the tumor cells using a grid. The mashed tissue was grown on gelatin-coated plates, in ES medium. Animal protocols were approved by the Institutional Animal Care and Use Committee of the Weizmann Institute of Science.
Immunohistochemistry of tumor sections.
Paraffin sections were deparaffinized using xylene and were rehydrated with alcohol series. The tissue was permeabilized using 0.5% Triton for 5 min. After three consecutive washes with PBS, the tissue was blocked using 3% BSA and 0.1% Triton X-100 in PBS for 60 min. The sections were stained with a polyclonal anti-p53 antibody (prepared in our laboratory), overnight at room temperature. After three consecutive washes with PBS, the secondary antibody was added for 60 min at room temperature, washed with PBS, and the signal was detected using DAB (Sigma-Aldrich) for 10 s. For counterstaining, sections were stained with hematoxylin. The sections were then dehydrated and mounted using xylene-based mounting medium.
Chimeric mice formation.
Chimeric mice were formed as described in Sarig et al. (1999).
Online supplemental material.
Figs. S1 and S2 describe the enhancement in the reprogramming process by either p53 KD or KO, respectively. Fig. S3 depicts the malignant feature of selected clones by showing their invasive growth patterns compared with the noninvasive growth of benign tumors. Fig. S4 describes the change in morphology of late-passage p53 KO and mut-p53 clones. Fig. S5 further shows the GOF of mut-p53 in reprogramming of MEFs using only Oct4 and Sox2. Fig. S6 is a graphical summary of the results. Table S1 summarizes the various cell types used in this study and their tumorigenic potential. Table S2 summarizes the karyotype analysis of selected clones. Table S3 is a list of primers used in this study.
Acknowledgments
We thank G. Lozano for her generosity in making the p53 mutant mice available.
This study was supported by a Center of Excellence grant from the Flight-Attendant Medical Research Institute, a grant from the Israel Science Foundation, and a grant from the Israel Cancer Research Fund. V. Rotter is the incumbent of the Norman and Helen Asher Professorial Chair for Cancer Research at the Weizmann Institute.
The authors claim no commercial interest in this study.
References
Author notes
R. Sarig and N. Rivlin contributed equally to this paper.


![Figure 1. The efficiency of reprogramming with three factors is enhanced by p53R172H. (A, Left) WT p53, p53 KO, and p53R172H MEFs were infected with retroviruses encoding Oct4, Sox2, and Klf4 (three factors) and assayed for AP activity. Numbers indicate the mean amount of AP-positive colonies ± SE, obtained from duplicate plates. (A, Right) Clones with ES-like morphology were analyzed for Nanog expression by quantitative real-time PCR (QRT-PCR) at the indicated time points. The chart shows the percentage of Nanog-positive clones. Upon appearance of Nanog-positive clones in a certain MEF type, we maintained only these clones. Hence, measurement of Nanog-positive percentage is not applicable (N/A) for later time points. (B) Nanog mRNA relative expression, measured by QRT-PCR, 4 wk after infection in selected p53 KO and p53R172H iPS clones. ESCs served as a positive control. Results indicate the mean ± SD of two duplicate runs. A representative experiment out of three independent infections is shown for A and B. (C) In vitro differentiation of representative p53 KO+3F and p53R172H+3F clones (#107 and #m-11, respectively) into the three germ layers: mesoderm (smooth muscle, stained with smooth muscle actin [SMA] antibody), ectoderm (neurons, stained with β-III-tubulin antibody), and endoderm (hepatic cells, stained with α-fetoprotein [AFP] antibody). Bars, 50 µm. A representative experiment out of two is shown.](https://cdn.rupress.org/rup/content_public/journal/jem/207/10/10.1084_jem.20100797/5/m_jem_20100797_rgb_fig1.jpeg?Expires=1779219310&Signature=k6AxY7UxrxyAYSiODpj2beBckJDcR-f9ZClIJWxR-vH8u3C56FDQvV5551UFKILLc5FqFavKncdfnEwNSkWkgMbG8MH6tkjUs8s1VXZCDTEWvFISplqdY8NFlmh83XHAZTc8LpLxg9NewMGkjs-HmLezljFRkQ~KpIgfXxeP0jn23RCZpqEJbv~18TA4M0DJ2NgFRvRX8XQdpLGZt4gMh83LkuApymMFTPHQBPrAkhzqPo-ERFEbj2SraeoDKWFF5rtIxK9hcdq25jwsJjDXI35SLYBUqVskqdextZJHXghJN8DrnOr18BJxLeXCjNjw57kOMVFEWm~NEkPEnkEmxQ__&Key-Pair-Id=APKAIE5G5CRDK6RD3PGA)