The complement system plays an essential protective role in the initial defense against many microorganisms. Flavivirus NS1 is a secreted nonstructural glycoprotein that accumulates in blood, is displayed on the surface of infected cells, and has been hypothesized to have immune evasion functions. Herein, we demonstrate that dengue virus (DENV), West Nile virus (WNV), and yellow fever virus (YFV) NS1 attenuate classical and lectin pathway activation by directly interacting with C4. Binding of NS1 to C4 reduced C4b deposition and C3 convertase (C4b2a) activity. Although NS1 bound C4b, it lacked intrinsic cofactor activity to degrade C4b, and did not block C3 convertase formation or accelerate decay of the C3 and C5 convertases. Instead, NS1 enhanced C4 cleavage by recruiting and activating the complement-specific protease C1s. By binding C1s and C4 in a complex, NS1 promotes efficient degradation of C4 to C4b. Through this mechanism, NS1 protects DENV from complement-dependent neutralization in solution. These studies define a novel immune evasion mechanism for restricting complement control of microbial infection.
The complement system is an essential component of the innate immune response against microorganisms. It consists of a network of soluble and cell surface proteins that recognize and target pathogens. Complement activation controls viral infections through multiple mechanisms, including enhanced B and T cell priming, release of anaphylatoxins (C3a, C4a, and C5a) that recruit leukocytes to the site of infection, production of opsonins (C1q, mannose binding lectin [MBL], C4b, and C3b) that bind viral particles, and formation of C5b-9 membrane attack complexes that lyse virions and/or infected cells (for review see Avirutnan et al., 2008). In response, viruses have evolved strategies to limit recognition by and activation of the complement cascade, including expression of surface proteins that bind the Fc domain of antibodies to prevent C1q-dependent complement activation, secretion of soluble viral proteins that mimic or recruit host complement regulators, direct incorporation of host complement control proteins on the virion, and up-regulation of complement regulatory proteins on the surface of infected cells (for review see Lambris et al., 2008).
Dengue virus (DENV) is a single-stranded positive sense enveloped RNA Flavivirus that is genetically related to several other major human pathogens, including West Nile virus (WNV) and yellow fever virus (YFV). DENV is a mosquito-transmitted pathogen that causes clinical syndromes in humans ranging from an acute self-limited febrile illness (dengue fever [DF]) to a severe and life-threatening vascular leakage and bleeding diathesis (dengue hemorrhagic fever/dengue shock syndrome [DHF/DSS]). Globally, DENV causes an estimated 50 million infections annually, resulting in 500,000 hospitalizations and ∼22,000 deaths (Morens and Fauci, 2008). Four serotypes of DENV circulate, and DHF/DSS is commonly associated with a secondary infection by a different serotype. Although antibody (Ab)-dependent enhancement of DENV infection in Fcγ receptor-bearing cells has been proposed to initiate pathogenesis (Halstead, 1988), the mechanism for how vascular leakage occurs remains uncertain. Cytopathic effects of virulent strains of DENV, a proinflammatory cytokine storm secondary to exuberant activation of poorly lytic cross-reactive T cells, and excessive complement activation have been suggested to contribute to the vascular leakage syndrome (for review see Clyde et al., 2006).
The 11-kb Flavivirus RNA genome encodes a polyprotein that is cleaved by viral and host proteases to generate three structural and seven nonstructural proteins. Flavivirus NS1 is a 48-kD nonstructural glycoprotein that is absent from the virion. NS1 is an essential gene as it is a required cofactor for the NS5 polymerase during viral RNA replication (Mackenzie et al., 1996; Lindenbach and Rice, 1997; Khromykh et al., 1999). In infected mammalian cells, NS1 is synthesized as a soluble monomer, dimerizes after posttranslational modification in the lumen of the endoplasmic reticulum, and is transported to the cell surface and accumulates extracellularly as higher order oligomers, including a hexamer (Flamand et al., 1999). Soluble NS1 also binds back to the plasma membrane of cells through interactions with specific sulfated glycosaminoglycans (Avirutnan et al., 2007). DENV NS1 has been implicated in the pathogenesis of DHF/DSS, although the mechanism remains uncertain. High levels of NS1 are detected in the serum of DENV-infected patients and correlate with severe disease (Libraty et al., 2002; Avirutnan et al., 2006). NS1 has been proposed to facilitate immune complex formation (Avirutnan et al., 2006); elicit autoantibodies that react with platelet and extracellular matrix proteins (Falconar, 1997) or damage endothelial cells via Ab-dependent, complement-mediated cytolysis (Lin et al., 2003); and directly enhance infection (Alcon-LePoder et al., 2005). Recently, WNV NS1 was shown to attenuate the alternative pathway of complement activation by binding the complement regulatory protein factor H (Chung et al., 2006a).
Here, we describe a novel immune evasion function of soluble Flavivirus NS1: specific inhibition of the classical and lectin pathway of complement activation through a direct interaction with C4 and C1s. DENV, WNV, and YFV NS1 all limit C4b deposition and classical and lectin pathway C3 convertase activity by enhancing cleavage of C4 through the recruitment of the complement-specific protease C1s.
RESULTS
DENV NS1 directly binds to C4/C4b and inhibits classical pathway (CP) activation
Based on a previous study with WNV NS1 (Chung et al., 2006a), we hypothesized that DENV NS1 might target the human complement system to attenuate the host immune response. An ELISA was used to screen for interactions between DENV NS1 and human complement proteins. Microtiter plates were adsorbed with purified human complement proteins (Fig. 1 and not depicted). Serum-free supernatants from baby hamster kidney (BHK) cells that stably propagate a DENV-2 subgenomic replicon (BHK-DENV2-Rep cells) and secrete high levels (up to 4 µg/ml) of NS1 (Avirutnan et al., 2007) and from control BHK cells were added to complement protein-coated wells. Bound DENV NS1 was detected using specific mAbs (Puttikhunt et al., 2003; Avirutnan et al., 2007). A strong interaction between DENV NS1 and C4 or C4b was identified (Fig. 1 A). Reciprocal co-immunoprecipitation experiments confirmed the NS1 and C4/C4b interaction (Fig. 1, B–E). However, the interaction of C4 or C4b and DENV NS1 is noncovalent, as the two proteins independently migrate at their expected sizes by electrophoresis and Western blot.
Direct binding of DENV NS1 to C4 and C4b. (A) ELISA. Microtiter plates were coated with BSA, C4, or C4b (5 µg/ml). After incubation with serum-free supernatants from BHK-DENV2-Rep cells or control BHK cells, bound DENV NS1 was detected using DENV NS1–specific mAbs. Data are the mean ± SD for three independent experiments. Asterisks denote NS1 binding that is statistically different from binding to background (**, P < 0.005; ***, P < 0.0005). (B–E) Reciprocal co-immunoprecipitation. Serum-free supernatants from BHK-DENV2-Rep or control BHK cells were incubated with purified C4 (B and D) or C4b (C and E; 20 µg/ml) and Western blots were performed after immunoprecipitation with anti-DENV NS1 mAb (2G6)–Sepharose (B and C) or anti–human C4–Sepharose (D and E). Immunoprecipitated material was probed with a goat polyclonal anti–human C4 Ab or DENV NS1–specific mAb (1F11), respectively. Subunits and cleavage fragments of C4 and C4b are labeled to the right of the gel; a 93-kD α chain of C4; 84-kD α′ chain of C4b; and 78-kD β chain of C4 and C4b. Notably, in the starting material of this C4 preparation, 20–30% was C4b. Western blot results are representative of two or three independent experiments.
Direct binding of DENV NS1 to C4 and C4b. (A) ELISA. Microtiter plates were coated with BSA, C4, or C4b (5 µg/ml). After incubation with serum-free supernatants from BHK-DENV2-Rep cells or control BHK cells, bound DENV NS1 was detected using DENV NS1–specific mAbs. Data are the mean ± SD for three independent experiments. Asterisks denote NS1 binding that is statistically different from binding to background (**, P < 0.005; ***, P < 0.0005). (B–E) Reciprocal co-immunoprecipitation. Serum-free supernatants from BHK-DENV2-Rep or control BHK cells were incubated with purified C4 (B and D) or C4b (C and E; 20 µg/ml) and Western blots were performed after immunoprecipitation with anti-DENV NS1 mAb (2G6)–Sepharose (B and C) or anti–human C4–Sepharose (D and E). Immunoprecipitated material was probed with a goat polyclonal anti–human C4 Ab or DENV NS1–specific mAb (1F11), respectively. Subunits and cleavage fragments of C4 and C4b are labeled to the right of the gel; a 93-kD α chain of C4; 84-kD α′ chain of C4b; and 78-kD β chain of C4 and C4b. Notably, in the starting material of this C4 preparation, 20–30% was C4b. Western blot results are representative of two or three independent experiments.
The functional significance of the NS1–C4 interaction was demonstrated in sheep erythrocyte (E) hemolysis assays in which the CP was activated by rabbit anti–sheep polyclonal Abs (Fig. 2). Each purified complement component was sequentially added to Ab-sensitized E (EA) in the presence or absence of DENV NS1. Preincubation of purified DENV NS1 with human C4, but not with C1, C2, or C3 (unpublished data) interfered with hemolysis in three different assays in which the complement proteins were limiting: (a) addition of purified components C1, C4, and C2 to EA (EAC14b2a) followed by an incubation with a 20-fold dilution of guinea pig serum (GPS) as the source of C3 and terminal complement components (C5-C9) in an EDTA containing buffer (GPS-EDTA; Fig. 2 A); (b) sequential addition of purified human C1-C9 to EA, in which purified C3-C9 was added to EAC14b2a instead of GPS-EDTA (Fig. 2 B); and (c) a single-step hemolysis assay in which EA were incubated with an 80-fold dilution of C4-deficient GPS supplemented with human C4 that had been preincubated in the presence or absence of DENV NS1 (Fig. 2 C). The specificity of DENV NS1 for inhibiting hemolytic activity was confirmed in preclearance experiments (Fig. S1 A) as follows: preincubation of DENV NS1 with anti-NS1 (2G6)– but not anti-E (4G2)–Sepharose abolished the inhibitory effect (Fig. S1 B). Notably, the amount and inhibitory activity of DENV NS1 after the preclearing step with 4G2–Sepharose was similar to that observed with a 1:2 dilution of starting material. The concentrations of NS1 used in these studies have been observed in plasma and pleural fluid of human patients infected with severe DENV infection (Alcon et al., 2002; Libraty et al., 2002; Avirutnan et al., 2006). Collectively, these functional experiments suggest that DENV NS1 specifically inhibits CP-induced lysis of targets via an interaction with C4.
DENV NS1 inhibits C4 to prevent CP dependent hemolysis. (A and B) Human C4 was incubated in the presence or absence of DENV NS1 and then added to sensitized EA bearing C1 (EAC1). After three washes, the EAC14b cells were incubated with purified C2, washed, and incubated with GPS treated with EDTA (A) or purified human components (B; C3-C9) at 37°C for 30 min. After centrifugation, the supernatant was analyzed by spectrophotometry at 414 nm. (C) Single-step hemolysis assay. EA were incubated with an 80-fold dilution of C4-deficient GPS that was supplemented with human C4, with or without preincubation with DENV NS1. The data represent the mean ± SD for three independent experiments. Asterisks denote hemolysis conditions that are statistically different from untreated cells (*, P < 0.05; **, P < 0.005; ***, P < 0.0005).
DENV NS1 inhibits C4 to prevent CP dependent hemolysis. (A and B) Human C4 was incubated in the presence or absence of DENV NS1 and then added to sensitized EA bearing C1 (EAC1). After three washes, the EAC14b cells were incubated with purified C2, washed, and incubated with GPS treated with EDTA (A) or purified human components (B; C3-C9) at 37°C for 30 min. After centrifugation, the supernatant was analyzed by spectrophotometry at 414 nm. (C) Single-step hemolysis assay. EA were incubated with an 80-fold dilution of C4-deficient GPS that was supplemented with human C4, with or without preincubation with DENV NS1. The data represent the mean ± SD for three independent experiments. Asterisks denote hemolysis conditions that are statistically different from untreated cells (*, P < 0.05; **, P < 0.005; ***, P < 0.0005).
DENV NS1 reduces CP C4b deposition
Next, we confirmed the complement inhibitory activity of DENV NS1 by measuring C4b and C3b deposition on the surface of EA. Pre-incubation of DENV NS1 with human C4 reduced C4b and C3b deposition in a dose-dependent manner (Fig. 3) and prevented cell lysis (Fig. 2, A–C). As expected, equivalent amounts of the control protein (BSA) did not interfere with C4b and C3b deposition (Fig. 3). To test if soluble NS1 also attenuates complement deposition on the cell surface of nucleated mammalian cells, we used an established Chinese hamster ovary (CHO) cell model system of complement activation (Barilla-LaBarca et al., 2002; Liszewski et al., 2008). Cells were sensitized with a polyclonal Ab against CHO cell surface antigens and the magnitude of C4b and C3b deposition was monitored by flow cytometry. Purified human CP complement components (C1, C4, C2, and C3) were preincubated with DENV NS1 in solution and subsequently added to Ab-sensitized CHO cells. As expected, DENV NS1 but not BSA decreased the amount of C4b and C3b deposited on the CHO cell surface (Fig. 3, E and F).
DENV NS1 reduces C4b and C3b deposition on the surface of cells. Human C4 was incubated with serially diluted purified DENV NS1 or BSA (12.5, 25, or 50 µg/ml) for 1 h before adding EAC1. After a 15-min incubation at 30°C, EAC14b were sequentially incubated with C2 and C3. After three washes, the deposition of C4b (A and C) and C3b (B and D) was determined by incubating EAC14b2a3b with anti-C4c or anti-C3c mAb, and analyzed by flow cytometry. Examples of histogram profiles in which DENV NS1, but not BSA, blocks C4b (A) and C3b (B) deposition are depicted. In C and D, data are expressed as the specific mean fluorescence intensity (MFI) of staining. The error bars indicate SD corresponding to three independent experiments. Asterisks denote C4b or C3b deposition that is statistically different from untreated cells (*, P < 0.05; **, P < 0.005; ***, P < 0.0005). (E and F) Soluble DENV NS1 restricts complement deposition on the surface of nucleated cells. CHO cells were sensitized with rabbit anti-CHO surface antigen IgG before incubation with the mixture of DENV NS1 or BSA (25 µg/ml) and purified human CP complement components C1, C4, C2, and C3, followed by immunostaining with murine mAb to human C4d (E) and C3d (F) and analyzed by flow cytometry. EDTA (20 mM) was added to inhibit complement activation for negative controls. Examples of histogram profiles from three independent experiments in which DENV NS1, but not BSA, restricted C4b (E) and C3b (F) deposition are shown.
DENV NS1 reduces C4b and C3b deposition on the surface of cells. Human C4 was incubated with serially diluted purified DENV NS1 or BSA (12.5, 25, or 50 µg/ml) for 1 h before adding EAC1. After a 15-min incubation at 30°C, EAC14b were sequentially incubated with C2 and C3. After three washes, the deposition of C4b (A and C) and C3b (B and D) was determined by incubating EAC14b2a3b with anti-C4c or anti-C3c mAb, and analyzed by flow cytometry. Examples of histogram profiles in which DENV NS1, but not BSA, blocks C4b (A) and C3b (B) deposition are depicted. In C and D, data are expressed as the specific mean fluorescence intensity (MFI) of staining. The error bars indicate SD corresponding to three independent experiments. Asterisks denote C4b or C3b deposition that is statistically different from untreated cells (*, P < 0.05; **, P < 0.005; ***, P < 0.0005). (E and F) Soluble DENV NS1 restricts complement deposition on the surface of nucleated cells. CHO cells were sensitized with rabbit anti-CHO surface antigen IgG before incubation with the mixture of DENV NS1 or BSA (25 µg/ml) and purified human CP complement components C1, C4, C2, and C3, followed by immunostaining with murine mAb to human C4d (E) and C3d (F) and analyzed by flow cytometry. EDTA (20 mM) was added to inhibit complement activation for negative controls. Examples of histogram profiles from three independent experiments in which DENV NS1, but not BSA, restricted C4b (E) and C3b (F) deposition are shown.
Based on the above experiments, DENV NS1 down-modulated CP-induced lysis of EA via a direct interaction with C4 through one of several possible mechanisms: (a) inhibiting C4 cleavage by C1; (b) preventing C4b attachment to the target cell surface; (c) preventing the CP convertase assembly; (d) inhibiting CP convertase formation and stability; or (e) promoting C4 degradation in solution.
DENV NS1 lacks the ability to regulate the CP convertases
A common mechanism for pathogens to evade human complement is to inactivate the central proteolytic enzymes, the C3 and C5 convertases (point c and d in the previous section; Lambris et al., 2008). To test whether DENV NS1 had this activity, we again used a hemolysis assay. In contrast to a soluble complement regulator, C4 binding protein (C4BP), which interferes with CP convertase assembly (Gigli et al., 1979), incubation of DENV NS1 with C1- and C4-treated EA (EAC14b) before adding C2 did not inhibit hemolysis (Figs. S1 and S2 A). The same result was obtained if CP C3 (C4b2a) or C5 (C4b2a3b) convertase was used; thus, incubation with DENV NS1 did not alter lytic activity whereas addition of the human regulators soluble complement receptor 1 (sCR1) and C4BP readily dissociated the convertases and inhibited the CP-induced hemolysis (Fig. S2, B and C). Therefore, although DENV NS1 binds C4b, it does not prevent convertase assembly or possess decay-accelerating activity.
DENV NS1 lacks cofactor activity for factor I to degrade C4b
Experiments were performed in the fluid phase to test whether NS1-modulated cofactor activity by augmenting the ability of factor I to degrade C4b in solution. Purified DENV NS1 was incubated with C4b, followed by sequential addition of factor I, with or without a known cofactor. Subsequently, C4b cleavage products were identified by Western blot using anti–C4d-specific mAbs. In contrast to the established cofactors C4BP, membrane cofactor protein (MCP), and CR1, addition of DENV NS1 did not enhance the protease activity of factor I for C4b; thus, NS1 lacks intrinsic cofactor activity for factor I (Fig. S3).
WNV NS1 also inhibits CP activation via a direct interaction with C4
We extended our study to test whether other Flavivirus NS1 proteins retained this complement inhibitory function. Notably, WNV and YFV NS1 efficiently bound human C4 and C4b (Fig. 4 A), but only WNV NS1 inhibited CP activation to a similar extent compared with DENV NS1 (Fig. 4 B).Inhibition of CP activation and complement-dependent hemolysis by DENV and WNV NS1 was observed with C4 from guinea pig (Fig. 4 C) or human serum (Fig. 4 D).
DENV and WNV NS1 inhibit CP activation via a direct interaction with C4. (A) DENV, WNV, and YFV NS1 interact with human C4/C4b. Microtiter plates were coated with BSA, C4, or C4b (5 µg/ml). After incubation with purified DENV, WNV, or YFV NS1 (5 µg/ml), bound NS1 was detected using DENV, WNV, or YFV NS1-specific mAbs. (B) EA were incubated with a 160-fold dilution of C4-deficient GPS that was supplemented with purified human C4 (63 ng/ml), with or without preincubation with DENV, WNV, or YFV NS1 or BSA (12.5–50 µg/ml). (C and D) DENV and WNV NS1 inhibit C4-mediated CP in guinea pig and human sera. EA were incubated with a 160-fold dilution of C4-deficient GPS that was supplemented with the indicated dilutions of fresh guinea pig (C) or human serum (D), with or without preincubation with DENV or WNV NS1 (50 µg/ml). Data are the mean ± SD for three independent experiments. Asterisks denote NS1 binding that is statistically different from binding to background (A) or hemolysis conditions which are statistically different from untreated cells (B–D; *, P < 0.05; **, P < 0.005; ***, P < 0.0005).
DENV and WNV NS1 inhibit CP activation via a direct interaction with C4. (A) DENV, WNV, and YFV NS1 interact with human C4/C4b. Microtiter plates were coated with BSA, C4, or C4b (5 µg/ml). After incubation with purified DENV, WNV, or YFV NS1 (5 µg/ml), bound NS1 was detected using DENV, WNV, or YFV NS1-specific mAbs. (B) EA were incubated with a 160-fold dilution of C4-deficient GPS that was supplemented with purified human C4 (63 ng/ml), with or without preincubation with DENV, WNV, or YFV NS1 or BSA (12.5–50 µg/ml). (C and D) DENV and WNV NS1 inhibit C4-mediated CP in guinea pig and human sera. EA were incubated with a 160-fold dilution of C4-deficient GPS that was supplemented with the indicated dilutions of fresh guinea pig (C) or human serum (D), with or without preincubation with DENV or WNV NS1 (50 µg/ml). Data are the mean ± SD for three independent experiments. Asterisks denote NS1 binding that is statistically different from binding to background (A) or hemolysis conditions which are statistically different from untreated cells (B–D; *, P < 0.05; **, P < 0.005; ***, P < 0.0005).
DENV and WNV NS1 promote cleavage of hemolytically active C4
To determine the mechanism for how NS1 inhibits CP-mediated complement activation, we assessed the efficiency of C4 cleavage by C1s in the fluid phase in the presence and absence of NS1. The ratio of the α and α′ chain of C4 and C4b was analyzed by Western blot. If NS1 acted by inhibiting C4 cleavage by C1s, we would expect greater amounts of C4-α compared with C4b-α′ chain. Instead, preincubation of DENV NS1 with C4, before addition of C1s, increased the generation of the C4b-α′ chain (Fig. 5 A). This result was initially surprising to us because, if NS1 promoted C4b-α′ chain accumulation on the erythrocyte cell surface, it should have enhanced hemolysis. However, a loss of C4-α chain and accumulation of C4b α′ chain was also observed in the absence of C1s when C4 was incubated with WNV NS1 but not with control proteins, BSA or lysozyme (Fig. 5 A); thus, NS1-dependent C4 cleavage in the fluid phase was analogous to that observed with C1s (Fig. 5 B). Cleavage of C4 in the presence of NS1 was also confirmed by detection of the small fragment C4a (Fig. 5 C). Nonetheless, C4 cleavage in the presence of NS1 was specific; incubation of purified C3 with NS1 did not result in degradation of the C3 α chain, even after prolonged incubation at 37°C (Fig. S4).
Purified DENV NS1 and WNV NS1 promote C4 cleavage. (A and B) Western blot analysis. (A) Purified DENV NS1, WNV NS1, BSA, or lysozyme (50 µg/ml) was preincubated with C4 (6.25 µg/ml) for 1 h on ice. Subsequently, the NS1-C4, BSA-C4, and lysozyme-C4 solutions were incubated at 30°C for 15 min. (B) Purified C4 was incubated with C1s (12 µg/ml) for 1 h at 30°C. Subunits and cleavage fragments of C4 and C4b are labeled to the right of the gel; 93 kD α chain of C4; 84 kD α′ chain of C4b. (C and D) Inhibition of C4 cleavage in the presence of NS1 by C1 inhibitor (C1-INH). (C) C4a ELISA. C4 was incubated with purified DENV NS1 or lysozyme (30 µg/ml) in the presence or absence of C1-INH (1.4 µg/ml) on ice for 1 h. (D) Single-step hemolysis assay. EA were incubated with a 160-fold dilution of C4-deficient GPS supplemented with human C4 (0.1 µg/ml) that was preincubated with DENV or WNV NS1 (30 µg/ml) in the presence or absence of C1-INH (40 µg/ml). In some experiments, C1 inhibitor (C1-INH; 40 µg/ml) was added to before the incubation with EA- and C4-deficient GPS. Data are the mean ± SD for four independent experiments. Asterisks denote C4a liberation (C) as measured by ELISA that is statistically different (**, P < 0.005) or hemolysis conditions (D) that are statistically different from untreated cells (***, P < 0.0005).
Purified DENV NS1 and WNV NS1 promote C4 cleavage. (A and B) Western blot analysis. (A) Purified DENV NS1, WNV NS1, BSA, or lysozyme (50 µg/ml) was preincubated with C4 (6.25 µg/ml) for 1 h on ice. Subsequently, the NS1-C4, BSA-C4, and lysozyme-C4 solutions were incubated at 30°C for 15 min. (B) Purified C4 was incubated with C1s (12 µg/ml) for 1 h at 30°C. Subunits and cleavage fragments of C4 and C4b are labeled to the right of the gel; 93 kD α chain of C4; 84 kD α′ chain of C4b. (C and D) Inhibition of C4 cleavage in the presence of NS1 by C1 inhibitor (C1-INH). (C) C4a ELISA. C4 was incubated with purified DENV NS1 or lysozyme (30 µg/ml) in the presence or absence of C1-INH (1.4 µg/ml) on ice for 1 h. (D) Single-step hemolysis assay. EA were incubated with a 160-fold dilution of C4-deficient GPS supplemented with human C4 (0.1 µg/ml) that was preincubated with DENV or WNV NS1 (30 µg/ml) in the presence or absence of C1-INH (40 µg/ml). In some experiments, C1 inhibitor (C1-INH; 40 µg/ml) was added to before the incubation with EA- and C4-deficient GPS. Data are the mean ± SD for four independent experiments. Asterisks denote C4a liberation (C) as measured by ELISA that is statistically different (**, P < 0.005) or hemolysis conditions (D) that are statistically different from untreated cells (***, P < 0.0005).
Because NS1 sequence does not encode any known protease motifs, one possibility was that the C4 but not C3 cleavage activity was caused by C4-specific proteases that copurified with NS1. To evaluate this, we assayed whether protease inhibitors could block NS1-dependent cleavage of C4. Among the protease inhibitors tested including phenylmethylsulfonylfluoride and commercial protease inhibitor cocktails (data not shown), the NS1-dependent C4b α′ chain accumulation was most efficiently inhibited by the plasma serine protease inhibitor, C1 inhibitor (C1-INH; Fig. 5 C). Correspondingly, C1-INH also abrogated C4 inhibitory activity of WNV and DENV NS1 in hemolysis assays (Fig. 5 D).
C1s/C1s proenzyme copurifies with WNV and DENV NS1
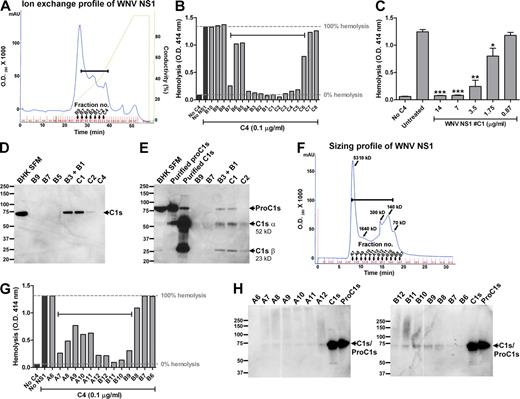
Because the complement protease C1s is blocked by C1-INH (Ziccardi, 1982) and is synthesized and secreted by a variety of cell types (Thielens and Arlaud, 2000), we evaluated whether hamster (from BHK cells) C1s copurified with NS1. Initially, a two-step purification was performed to generate highly purified preparations of NS1 (Avirutnan et al., 2007). The elution profile of affinity-purified WNV NS1 (first column) followed by ion-exchange (second) column displays a heterogeneous profile (Fig. 6 A), which is likely caused by the presence of oligomers of soluble NS1 (Flamand et al., 1999; Fig. S5). The heterogeneity in size was confirmed by size exclusion chromatography (Fig. 6 F and Fig. S6). After purification, each fraction of NS1 was tested for C4 inhibitory activity in the hemolysis assay, as well as the presence of hamster C1s by Western blot with a cross-reactive anti–human C1s polyclonal Ab. After separation by ion-exchange chromatography, all fractions of WNV NS1 had C4 inhibitory activity, with the exception of the main peak fractions (B8-B10; Fig. 6 B). In our functional experiments (Figs. 2–5,345), high concentrations of NS1 (20–50 µg/ml) were required to inhibit hemolysis. However, when the fraction with peak activity (fraction C1; Fig. 6, A and B) was serially diluted and subjected to the C4 hemolysis assay, the specific C4 inhibitory activity was observed at a much lower concentration of NS1 (1.75 µg/ml; Fig. 6 C). Hamster C1s was detected in most of the fractions of purified WNV NS1 that had C4 inhibitory activity, but not in the NS1 fractions that lacked activity (Fig. 6 D). Correspondingly, the fractions of WNV NS1 after size exclusion chromatography that exhibited inhibitory activity in the C4 hemolysis assay (Fig. 6, F and G) also had detectable levels of C1s (Fig. 6 H). Although similar results were observed with DENV NS1, hamster C1s was not detected in purified fractions of YFV NS1 (not depicted); consistent with this, YFV NS1 bound C4, but did not inhibit in the hemolysis assay (Fig. 4 B).
C1s/proC1s copurifies with NS1. (A) Two-step purification of WNV NS1. Immunoaffinity-purified WNV NS1 was passed over an ion-exchange column, and NS1 was eluted with a linear NaCl gradient (diagonal line). Silver stain and Western blot of each fraction were performed (Fig. S5 and not depicted). All fractions were tested for C4 inhibitory activity in a single-step hemolysis assay (B). C4 (0.1 µg/ml) was preincubated with an individual concentrated fraction (25 µl) before the addition of EA- and C4-deficient GPS (1:160). Fractions with C4 inhibitory activity are bracketed (A and B). (C) WNV NS1 fraction #C1 from ion exchange chromatography was twofold serially diluted and subjected to a single-step C4 hemolysis assay. (D and E) Western blot analysis for C1s/proC1s from ion exchange fractions shown in A. (D) Nonreduced SDS-PAGE. Lane 1, 100-fold concentrated serum-free culture supernatants (SFM) of BHK cells; lanes 2–7, 10-fold concentrated purified WNV NS1 fractions after ion-exchange chromatography. The proteins were separated on a 4–12% gradient nonreduced SDS-PAGE, transferred, and probed with a goat anti–human C1s serum. The anti–human C1s Ab cross-reacts with hamster C1s. (E) SDS-PAGE, reducing conditions. Lane 1, 100-fold concentrated SFM of BHK cells; lanes 2 and 3, purified human C1s (huC1s) and human proC1s (huProC1s; 10 ng); lanes 4–8, 10-fold concentrated purified WNV NS1 fractions after ion-exchange chromatography. (F) Size exclusion chromatography profile of affinity-purified WNV NS1. Molecular sizes of indicated fractions were calculated from a set of protein standards loaded on the same column. (G) Size exclusion chromatography fractions were collected, concentrated 10-fold, and subjected to a single-step hemolysis assay as described in B, as well as a nonreduced SDS-PAGE and Western blot with anti–human C1s Ab (H). Brackets denote the fractions that inhibit C4-dependent hemolysis (F and G). Results are representative of two or three independent experiments.
C1s/proC1s copurifies with NS1. (A) Two-step purification of WNV NS1. Immunoaffinity-purified WNV NS1 was passed over an ion-exchange column, and NS1 was eluted with a linear NaCl gradient (diagonal line). Silver stain and Western blot of each fraction were performed (Fig. S5 and not depicted). All fractions were tested for C4 inhibitory activity in a single-step hemolysis assay (B). C4 (0.1 µg/ml) was preincubated with an individual concentrated fraction (25 µl) before the addition of EA- and C4-deficient GPS (1:160). Fractions with C4 inhibitory activity are bracketed (A and B). (C) WNV NS1 fraction #C1 from ion exchange chromatography was twofold serially diluted and subjected to a single-step C4 hemolysis assay. (D and E) Western blot analysis for C1s/proC1s from ion exchange fractions shown in A. (D) Nonreduced SDS-PAGE. Lane 1, 100-fold concentrated serum-free culture supernatants (SFM) of BHK cells; lanes 2–7, 10-fold concentrated purified WNV NS1 fractions after ion-exchange chromatography. The proteins were separated on a 4–12% gradient nonreduced SDS-PAGE, transferred, and probed with a goat anti–human C1s serum. The anti–human C1s Ab cross-reacts with hamster C1s. (E) SDS-PAGE, reducing conditions. Lane 1, 100-fold concentrated SFM of BHK cells; lanes 2 and 3, purified human C1s (huC1s) and human proC1s (huProC1s; 10 ng); lanes 4–8, 10-fold concentrated purified WNV NS1 fractions after ion-exchange chromatography. (F) Size exclusion chromatography profile of affinity-purified WNV NS1. Molecular sizes of indicated fractions were calculated from a set of protein standards loaded on the same column. (G) Size exclusion chromatography fractions were collected, concentrated 10-fold, and subjected to a single-step hemolysis assay as described in B, as well as a nonreduced SDS-PAGE and Western blot with anti–human C1s Ab (H). Brackets denote the fractions that inhibit C4-dependent hemolysis (F and G). Results are representative of two or three independent experiments.
C1s is synthesized as a single 80-kD chain proenzyme (proC1s) and activated after cleavage of a single peptide bond between amino acids R437 and I438, yielding a disulfide-linked 52-kD α chain and 28- kD β chain (Thielens and Arlaud, 2000). Reducing SDS-PAGE and Western blot analysis of the hamster C1s that copurified with NS1 revealed three distinct bands corresponding to the α and β chains of activated C1s and proC1s. In contrast, only a single band of proC1s was observed in a concentrated (100-fold) serum-free culture supernatant from uninfected BHK cells (Fig. 6 E). Autocatalytic activation of proC1s independent of its activator C1r has been previously shown (Morgan and Nair, 1975). ProC1s may have become auto-activated during the purification process or alternatively, binding of NS1 to proC1s induced autocatalysis.
Flavivirus NS1 directly binds C1s/C1s proenzyme and enhances cleavage of C4
As our data suggested a separate biochemical interaction between NS1 and C1s, experiments were performed to test if NS1 physically interacted with C1s and C1s proenzyme. Purified human proC1s, WNV NS1, or mixtures of both were separated by size exclusion chromatography. When proC1s was run alone, Western blot analysis showed that it was present exclusively in fractions B9 and B10 (Fig. 7 A). When the same amount of proC1s was preincubated with WNV NS1, it distributed more broadly over the fractions that contain WNV NS1 (Fig. 7, B and C). Importantly, the distribution of a Fab fragment of similar size but irrelevant specificity did not change when mixed with WNV NS1 (Fig. 7, D and E). Additionally, a change in the distribution pattern of size exclusion chromatography fractions that contained WNV NS1 after binding to human proC1s was also observed (Fig. 7, C and F, and Fig. S6 B), suggesting an avid interaction. Based on the column migration patterns, we postulated a direct interaction between NS1 and C1s/proC1s. Binding assays confirmed that DENV, WNV, and YFV NS1 directly interacted with human C1s and proC1s (Fig. 7, G and H).
Flavivirus NS1 directly binds to C1s/proC1s. (A–F) Size-exclusion chromatography. Purified huProC1s (A) or Fab fragment of murine mAb to WNV E (E9-Fab; D) or the mixture of huProC1s + WNV NS1 (B and C) or E9-Fab + WNV NS1 (E and F) were fractionated by size exclusion chromatography. Fractions were concentrated 10-fold, separated on SDS-PAGE under reducing (A–C) or nonreducing (D–F) conditions and immunoblotted with goat antiserum to huC1s (A and B), goat anti–mouse IgG (D and E), or mouse anti-WNV NS1 (C and F). Subunits of C1s are labeled to the right of the gel; an 85-kD subunit of huProC1s or huC1s; a 52-kD α chain of huC1s; and a 23-kD β chain of huC1s. Of note, a subset of proC1s was activated during the fractionation to become C1s (A and B). Results are representative of two independent experiments. (G and H) ELISA. Microtiter plates were coated with purified BSA and huC1s (G) or BSA and huProC1s (H). After incubation with affinity-purified DENV, WNV, or YFV NS1, bound NS1 was detected using DENV-, WNV-, or YFV NS1–specific mAbs, respectively. Specific binding was calculated by subtracting the OD in antigen-coated wells from the OD. in BSA-coated wells. Data are presented as the mean ± SD for three independent experiments.
Flavivirus NS1 directly binds to C1s/proC1s. (A–F) Size-exclusion chromatography. Purified huProC1s (A) or Fab fragment of murine mAb to WNV E (E9-Fab; D) or the mixture of huProC1s + WNV NS1 (B and C) or E9-Fab + WNV NS1 (E and F) were fractionated by size exclusion chromatography. Fractions were concentrated 10-fold, separated on SDS-PAGE under reducing (A–C) or nonreducing (D–F) conditions and immunoblotted with goat antiserum to huC1s (A and B), goat anti–mouse IgG (D and E), or mouse anti-WNV NS1 (C and F). Subunits of C1s are labeled to the right of the gel; an 85-kD subunit of huProC1s or huC1s; a 52-kD α chain of huC1s; and a 23-kD β chain of huC1s. Of note, a subset of proC1s was activated during the fractionation to become C1s (A and B). Results are representative of two independent experiments. (G and H) ELISA. Microtiter plates were coated with purified BSA and huC1s (G) or BSA and huProC1s (H). After incubation with affinity-purified DENV, WNV, or YFV NS1, bound NS1 was detected using DENV-, WNV-, or YFV NS1–specific mAbs, respectively. Specific binding was calculated by subtracting the OD in antigen-coated wells from the OD. in BSA-coated wells. Data are presented as the mean ± SD for three independent experiments.
Although all of our experiments suggested that NS1 could interact with both C4 and C1s to limit complement activation, an underlying concern was that the interaction with C1s was still nonspecific. We reasoned that a nonspecific interaction should not affect the inherent enzymatic activity of C1s. However, if NS1 enhanced the C4 cleavage activity of C1s, it would strongly support the concept of a specific functional interaction. We evaluated this hypothesis using a modified hemolysis assay. Purified NS1 was preincubated with human C1s or proC1s before the addition of human C4; subsequently, C4-deficient GPS was added to sensitized sheep EA. Higher concentrations of C4 were used in this assay compared with the previous hemolysis experiments to overcome the inherent C4 cleavage activity of hamster C1s/proC1s that copurified with WNV and DENV NS1. Notably, WNV and DENV NS1, but not BSA or lysozyme, enhanced the activity of C1s and proC1s to cleave C4 as observed by decreased hemolysis (Fig. 8, A and B). Most importantly, although purified YFV NS1 did not associate significantly with hamster C1s/proC1s to promote degradation of C4 by itself (Fig. 4 B), it readily bound human C1s/proC1s (Fig. 7, G and H), which then facilitated cleavage of C4 (Fig. 8, A and B) in a manner similar to WNV and DENV NS1. Acceleration of C4 degradation in solution by human proC1s in the presence of YFV NS1 was confirmed in kinetic experiments (Fig. 8 C). This activity was specific to NS1, as lysozyme or BSA did not alter the kinetics of C4 cleavage by proC1s (Fig. 8 C and not depicted).
Flavivirus NS1 enhances ability of C1s and proC1s to cleave C4. Purified WNV, DENV, or YFV NS1 (20 µg/ml) was incubated with huC1s (0.04 µg/ml; A) or huProC1s (0.4 µg/ml; B) on ice. After a 1-h incubation, C4 (5 µg/ml) was added and incubated for 1 h on ice followed by EA and 160-fold dilution of C4-deficient GPS. (C) YFV NS1 accelerates C4 degradation by proC1s. Purified YFV NS1 (20 µg/ml) was incubated with or without huProC1s (0.2 µg/ml) for 1 h on ice followed by the addition of C4 (2.5 µg/ml). At indicated times after incubation at room temperature, EA and 160-fold dilution of C4-deficient GPS were added and hemolysis was determined. The data represent the mean ± SD for three to four independent experiments. Asterisks denote hemolysis conditions that are statistically different from the cells treated with C1s or proC1s alone (*, P < 0.05; **, P < 0.005; ***, P < 0.0005).
Flavivirus NS1 enhances ability of C1s and proC1s to cleave C4. Purified WNV, DENV, or YFV NS1 (20 µg/ml) was incubated with huC1s (0.04 µg/ml; A) or huProC1s (0.4 µg/ml; B) on ice. After a 1-h incubation, C4 (5 µg/ml) was added and incubated for 1 h on ice followed by EA and 160-fold dilution of C4-deficient GPS. (C) YFV NS1 accelerates C4 degradation by proC1s. Purified YFV NS1 (20 µg/ml) was incubated with or without huProC1s (0.2 µg/ml) for 1 h on ice followed by the addition of C4 (2.5 µg/ml). At indicated times after incubation at room temperature, EA and 160-fold dilution of C4-deficient GPS were added and hemolysis was determined. The data represent the mean ± SD for three to four independent experiments. Asterisks denote hemolysis conditions that are statistically different from the cells treated with C1s or proC1s alone (*, P < 0.05; **, P < 0.005; ***, P < 0.0005).
NS1 protects Flaviviruses from complement attack
Complement can directly neutralize Flavivirus virions and infectivity (Mehlhop et al., 2005) in vitro and has a protective role in restricting WNV infection in mice. Because Flavivirus NS1 antagonizes C4 and subsequent C3 deposition, we hypothesized that soluble NS1 that accumulates to high amounts (up to 50 µg/ml) in serum (Alcon et al., 2002) could protect DENV from direct complement-mediated neutralization. As expected, DENV was efficiently neutralized by naive wild type GPS (Fig. 9 A). In contrast, C4-deficient GPS or heat-inactivated wild-type serum failed to diminish DENV infectivity, confirming a complement-dependent neutralization mechanism (Fig. 9, A and B). Addition of purified human C4 to guinea pig C4-deficient serum restored the ability to neutralize DENV infection in a dose-dependent manner (Fig. 9 B). Importantly, the addition of soluble DENV NS1 (Fig. 9 B) or WNV NS1 (not depicted), but not BSA, rescued infectivity. This antagonistic effect of NS1 was C4-dependent, as addition of higher concentrations of human C4 overcame the inhibition of GPS neutralization by NS1. Although one study suggested that pretreatment of cells with soluble DENV NS1 before infection of hepatoma cells improves virus yield twofold (Alcon-LePoder et al., 2005), we did not observe this phenomenon; when NS1 was added alone or mixed with heat-inactivated serum, no changes in infectivity were observed (Fig. 9 B and not depicted). Collectively, these studies demonstrate that soluble NS1 can antagonize C4 function, which affects viral infection.
Soluble NS1 protects DENV from complement attack. (A) Neutralization of DENV by GPS. DENV virions were incubated with untreated or heat-inactivated (HI) normal GPS for 1 h at 37°C to allow complement activation. The samples were then added to BHK-21 monolayer, and after agarose overlay, cultured for 5 d. After fixation and staining of wells, plaques were counted. (B) Soluble DENV NS1 protects DENV from complement C4-mediated neutralization. Purified human C4 at the indicated concentrations was incubated with soluble DENV NS1 or BSA (50 µg/ml) or buffer (PBS) alone for 1 h at room temperature. DENV was then added and followed by untreated or HI C4-deficient C4D GPS. Samples were incubated for 1 h at 37°C before infection of BHK-21 cells, as described in A. Data are representative of three independent experiments.
Soluble NS1 protects DENV from complement attack. (A) Neutralization of DENV by GPS. DENV virions were incubated with untreated or heat-inactivated (HI) normal GPS for 1 h at 37°C to allow complement activation. The samples were then added to BHK-21 monolayer, and after agarose overlay, cultured for 5 d. After fixation and staining of wells, plaques were counted. (B) Soluble DENV NS1 protects DENV from complement C4-mediated neutralization. Purified human C4 at the indicated concentrations was incubated with soluble DENV NS1 or BSA (50 µg/ml) or buffer (PBS) alone for 1 h at room temperature. DENV was then added and followed by untreated or HI C4-deficient C4D GPS. Samples were incubated for 1 h at 37°C before infection of BHK-21 cells, as described in A. Data are representative of three independent experiments.
DISCUSSION
Viruses have evolved strategies to avoid recognition and destruction by the complement system (for review see Lambris et al., 2008). WNV NS1 has previously been shown to attenuate alternative pathway activation by recruiting complement regulator factor H to facilitate C3b inactivation by factor I (Chung et al., 2006a). Herein, we define a novel mechanism in which NS1 restricts classical/lectin pathway activation by targeting C4. Binding of soluble NS1 to proC1s/C1s and C4 enhances the cleavage of C4 to C4b in solution, thus decreasing activation by the classical and lectin pathways. The interaction between Flavivirus NS1, C1s, and C4 has functional consequences, including reduced deposition of C3b and C4b on virions and target cells and protection of virus from complement-mediated neutralization.
The targeting of C4 in the context of an NS1 interaction with proC1s/C1s is a novel evasion strategy to attenuate classical and lectin pathway activation. Herpesviruses and coronaviruses interfere with CP activation by secreting or expressing decoy molecules with Fc receptor function (Oleszak et al., 1993; Para et al., 1982), whereas Porphyromonas, Streptococcus, and Staphylococcus bacteria degrade IgG and/or inhibit IgG interaction with C1q (Björck and Kronvall, 1984; Schenkein et al., 1995; von Pawel-Rammingen and Björck, 2003). Additionally, the Staphylococcus SCIN and Efb proteins block CP and alternative pathway C3 and C5 convertases (Rooijakkers et al., 2005; Jongerius et al., 2007). Mechanistically, NS1 promotes cleavage of C4 in solution, which attenuates generation of C3b and C5b-9 on targets (e.g., virions or virus-infected cells). An analogous cleavage of C3 to C3b-like proteins by extracellular gelatinase has been described as a mechanism of complement evasion by Enterococcus faecalis (Park et al., 2008). Our studies do not rule out the possibility that NS1 also inhibits complement activation by independently preventing C4b attachment to target cells. Unlike poxviruses, which express viral virulence factors with structural and functional similarities to human complement regulators (Rosengard et al., 2002), NS1 itself lacks any apparent sequence homology to known complement proteins or enzymes. Interestingly, C4 is the only complement protein that is sulfated on a tyrosine residue, and this posttranslational modification increases the efficiency of C4 cleavage by C1s (Hortin et al., 1989). As DENV NS1 binds sulfated glycosaminoglycans (Avirutnan et al., 2007), it is tempting to speculate that NS1 binding near the sulfated tyrosine on C4 could render it more susceptible to C1s or C1s-like proteases. Investigations with mutant NS1 proteins and C4 lacking sulfation are planned to directly test this hypothesis.
The presence of C4 protease activity (hamster C1s) in the WNV and DENV NS1 preparations initially raised the possibility of a contaminant. Several biochemical experiments, however, suggest that the interaction of Flavivirus NS1 with C1s and C4 is specific: (a) YFV NS1, which does not copurify efficiently with hamster C1s, binds C4 but lacks cleavage activity. However, addition of YFV NS1 to limiting quantities of human proC1s and C1s enhances the cleavage rate of C4; (b) WNV, YFV, and DENV NS1 all bind directly to human proC1s and C1s by ELISA; (c) WNV NS1 specifically shifts the size exclusion chromatography profile of human proC1s. Although our data suggest that NS1 promotes cleavage of C4 by recruiting and enhancing the enzymatic activity of C1s, it remains unclear mechanistically how NS1 achieves this. Binding of NS1 to C1s/proC1s may cause structural changes that increase the proteolytic activity of C1s. Alternatively, oligomeric forms of NS1 could bring C4 and C1s together for a sustained interaction that promotes cleavage.
Our data showing that NS1 inhibits the classical and lectin pathways of complement activation appears to contrast with previous experiments showing that DENV NS1 triggers accumulation of C5b-9 complexes in human serum (Avirutnan et al., 2006). This discrepancy may be explained by the presence of natural and neutralizing IgM against NS1 and the relative concentrations of NS1 and C4 in serum (comparatively low NS1 and high C4) that could attenuate an inhibitory effect on C4 activation. In peripheral tissues where the majority of Flavivirus infection occurs, higher local levels of NS1 coupled with lower levels of extravascular complement and Ab concentrations could efficiently inhibit C4 function. Flaviviruses, thus, may use NS1 to bind C1s proenzyme produced from the same infected cell or neighboring cells to inactivate C4 in solution. By forming a complex with C1s, NS1 can promote continuous cleavage of C4 to C4b. In solution, this nascently generated C4b would have only a few microseconds to bind to a target before further hydrolysis, as observed with activated C4b. Thus, NS1 targeting of C4 could directly limit opsonization and neutralization of virions and thereby facilitate local dissemination.
Complement activation has been implicated in the vascular leakage syndrome of severe DENV infection (Bokisch et al., 1973; Avirutnan et al., 2006) with C4 consumption occurring in patients with DHF/DSS (Bokisch et al., 1973). The NS1 antagonism of complement function could explain some of the clinical and pathological findings of severe DENV disease. However, severe dengue disease usually occurs after secondary DENV infection by a different viral serotype. Pre-existing cross-reactive anti-NS1 Abs could modulate (enhance or inhibit) the ability of DENV NS1 to attenuate complement activation during secondary infection. Such an interaction at endothelial or serosal sites could trigger dysfunctional complement responses by NS1-Ab immune complexes that promote fluid extravasation into pleural and peritoneal spaces, a characteristic of DHF/DSS (Nimmannitya, 1987). Alternatively, antagonism of C4 function by NS1 may have a more important role in primary Flavivirus infection by enhancing the infectivity of virus in serum or tissues, which otherwise can be neutralized by complement. An improved understanding of the novel immune evasion mechanisms of Flavivirus NS1 will likely foster insight into the host-pathogen interactions that modulate disease severity.
In summary, our results point to formation of a complex of soluble NS1 with human C1s and C4. This complex promotes cleavage by C1s of C4 to C4b and thereby limits the supply of native C4 to participate in complement activation at the infectious site. NS1 derived from at least three clinically important Flaviviruses, DENV, WNV, and YFV, possesses this immune evasion activity for the human complement system.
MATERIALS AND METHODS
Purified Flavivirus NS1 and complement proteins
DENV NS1 was produced and isolated as previously described from DENV2-infected mammalian cells and BHK-DENV2-Rep cells (Avirutnan et al., 2006, 2007). WNV and YFV NS1 were isolated from supernatants of BHK-WNV-Rep and BHK-YFV-Rep cells as previously described (Chung et al., 2006a; Patkar and Kuhn, 2008) or BHK cells infected with recombinant Sindbis viruses encoding Flavivirus NS1. WNV and YFV NS1 were expressed using the double subgenomic Sindbis virus 39 E2H55K50 (39HK; Ryman et al., 2007). In brief, the NS1 gene of WNV and YFV including a 24-amino acid signal sequence corresponding to the C-terminus of the E protein was amplified from infected Vero cells by RT-PCR using the following oligonucleotide primers (WNV NS1 forward 5′-GGGCGGCCGCACCATGGATAGGTCCATAGCTCTCACGTTT-3′; WNV NS1 reverse 5′-CTGCGGCCGCTAAGCATTCACTTGTGACTGCAC-3′; YFV NS1 forward 5′-GCGGCCGCACCATGGACATGACAATGTCCATGAGCA-3′; YFV NS1 reverse 5′-TCAAGCTGTAACCCAGGAGCGCACCAG-3′). WNV and YFV NS1 were subcloned into 39HK after digestion with NotI and PmeI restriction enzymes. After sequencing, recombinant 39HK expressing WNV or YFV NS1 (39HK WNV NS1 or 39HK YFV NS1) was produced by SP6 DNA-dependent RNA polymerase in vitro transcription. DNA templates linearized with XhoI were transcribed in vitro by SP6 RNA polymerase using mMESSAGE mMACHINE kit (Ambion) following the manufacturer’s instruction. In vitro–transcribed RNA was electroporated into BHK cells with 3 consecutive electrical pulses of 850 V at 25 µF and ∞ Ω using the Gene Pulser Xcell (Bio-Rad Laboratories) and double subgenomic infectious viruses were harvested 2 d later. WNV or YFV NS1 was harvested from supernatants of BHK cells infected with 39HK WNV NS1 or 39HK YFV NS1 at a multiplicity of infection (MOI) of 1 in serum-free DME at 36 h. Infectious recombinant Sindbis virus was inactivated by β-propiolactone treatment at 37°C overnight or NP-40 (0.05% [vol/vol] final concentration) before NS1 purification using a Flavivirus cross-reactive anti-NS1 (9NS1; Chung et al., 2006b) Sepharose 4B column. A two-step purification of Flavivirus NS1 was performed as described previously (Avirutnan et al., 2007) using ion exchange or size exclusion chromatography.
All purified human complement proteins were purchased commercially (Complement Technologies) unless otherwise stated. To differentiate between C1s and proC1s, SDS-PAGE and Western blot analysis were performed: under reducing (5% β-mercaptoethanol) conditions, C1s appears as two bands (52 kD α chain and 23 kD β chain), whereas proC1s migrates as an ∼80-kD single band (see Fig. 6 E). Under nonreducing conditions, C1s and proC1s both migrate as a single ∼80-kD band. For each preparation of proC1s, this type of analysis confirmed the purity of proC1s relative to C1s. Furthermore, in functional analyses, 10–100–fold more proC1s than C1s was required to cleave an equal quantity of C4.
NS1 and C4/C4b binding ELISA
Maxi-Sorp microtiter plates were adsorbed with purified C4 or C4b (5 µg/ml in PBS) at 4°C overnight. After five washes with PBS, nonspecific binding sites were blocked with 1% heat-inactivated BSA in PBS for 2 h at room temperature followed by five washes with PBS. Clarified (200 g, 5 min) serum-free supernatants from BHK or BHK-DENV2-Rep cells were added to each well and incubated for 2 h at room temperature. Plates were then washed five times with PBS containing 0.05% Tween-20 followed by a 1-h incubation with a mixture of DENV NS1-specific mAbs (1A4, 1B2, 1F11, 2G6, and 2E3; 1 µg/ml of each; Puttikhunt et al., 2003). After washing, biotinylated goat anti–mouse IgG and horseradish peroxidase (HRP)–conjugated streptavidin were added sequentially at room temperature. After six final washes with PBS, signal was detected by adding 3,3′, 5,5′-tetramethylbenzidine substrate. Plates were evaluated on a 96-well plate reader (GENois Pro; Tecan Instruments). In some experiments, purified NS1 from DENV and WNV (5 µg/ml) was used instead of crude supernatants. A mixture of WNV NS1–specific mAbs (10NS1, 14NS1, 16NS1, 17NS1, and 22NS1; (Chung et al., 2006b) was used to detect WNV NS1.
Immunoprecipitation and Western blot studies
NS1 immunoprecipitation.
NS1-containing supernatants were incubated with human C4 or C4b at 4°C overnight and then immunoprecipitated with anti-NS1 mAb (2G6)–Sepharose. After five washes, bound proteins were eluted in SDS reducing sample buffer and separated by 10% SDS-PAGE. Western blot was performed using goat anti–human C4 Ab (Quidel) and HRP-conjugated anti–goat IgG (GE Healthcare).
C4 immunoprecipitation.
NS1-containing supernatants were incubated with C4 and C4b and immunoprecipitation was performed with anti–human C4 Ab-coated beads. After five washes, the samples were boiled in SDS sample buffer and separated by 12% SDS-PAGE. Western blot was performed using anti-DENV NS1 mAb (1F11) hybridoma supernatant and HRP-conjugated anti–mouse IgG. Anti–human C4 Ab-coated beads were prepared by adding 5 µg of goat anti–human C4 polyclonal Ab (Abcam) to 50 µl of TrueBlot anti–goat Ig immunoprecipitation beads (eBioscience).
Erythrocyte hemolysis assay
The assay was performed by a stepwise buildup of complement intermediates on EA according to previous work (Krych-Goldberg et al., 1999). EA were incubated with C1 (EAC1) for 15 min at 30°C. Before addition to EAC1 cells, C4 was preincubated with purified DENV NS1 for 1 h on ice. After a 15-min incubation at 30°C, C1- and C4-treated EA (EAC14b) were washed three times and incubated with C2 for 4 min at room temperature. C1, C4, and C2 treated EA (EAC14b2) were washed and incubated with a 20-fold dilution of GPS in 40 mM EDTA containing veronal buffered saline (GPS-EDTA) for 30 min at 37°C. Alternatively, GPS-EDTA was replaced with buffer containing C3 and each terminal component (C5-C9). In a single-step hemolysis assay, EA were incubated with an 80- or 160-fold dilution of C4-deficient GPS supplemented with human C4 that was preincubated with DENV NS1 for 30 min at 37°C. In some experiments, C1 inhibitor (C1-INH; 40 µg/ml) was added to before the incubation with EA and C4-deficient GPS. After centrifugation, erythrocyte lysis was assayed in the supernatant by spectrophotometry at 414 nm.
For preclearing experiments DENV NS1 was incubated with anti-NS1 (2G6) or anti-E (4G2; negative control) Sepharose beads for 4 h at 4°C. The quantity of DENV NS1 after preclearing was analyzed by Western blot. The precleared solutions also were subjected to a single-step hemolysis assay.
The assay for decay-accelerating activity was performed essentially as previously described (Krych-Goldberg et al., 2005). To prepare the CP C3 convertase, EAC14b were incubated for 4 min at room temperature with C2; for the CP C5 convertase, cells were incubated under the same conditions with C2 and C3. EAC14b2a or EAC14b2a3b were incubated with purified DENV NS1, sCR1, or C4BP for 10 min at 30°C. Subsequently, GPS-EDTA was added and hemolysis was determined.
To test for the activity of Flavivirus NS1 to enhance C1s/proC1s activity, purified WNV, DENV, and YFV NS1 (20 µg/ml) was incubated with C1s (0.04 µg/ml) or proC1s (0.4 µg/ml) on ice. After a 1-h preincubation, C4 (4µg/ml) was added to the NS1-C1s/proC1s mixture and incubated for 1 h on ice. 50 µl of EA (8 × 106 cells) and 500 µl of a 160-fold dilution of C4-deficient GPS were added and incubated for 30 min at 37°C, and then hemolysis was determined. In some experiments, purified YFV NS1 (20 µg/ml) was incubated with proC1s (0.2 µg/ml) for 1 h on ice. Purified human C4 (2.5 µg/ml) was then added to NS1-proC1s mixture and incubated for 0, 5, 15, 30, 45, and 60 min at room temperature followed by the addition of EA- and C4-deficient GPS as described in the first paragraph of this section.
C4b cofactor activity assay
Purified soluble complement receptor-1 (sCR1) was a gift (H. Marsh, Avant Immunotherapeutics, Inc., Needham, MA). Recombinant MCP was generated as previously described (Liszewski et al., 2006). C4b was incubated with purified DENV NS1 or WNV NS1 or BSA for 1 h at 4°C. Subsequently, factor I, with or without a cofactor (C4BP or sCR1 or MCP), was added to the C4b-NS1 solution. After a 2-h incubation at 37°C, reducing sample buffer was added, and the fragments of C4b were separated on 10% SDS-PAGE. Western blot was performed using an anti-C4d mAb (Quidel) and a HRP-conjugated anti–mouse IgG.
C3b and C4b deposition on erythrocyte cell surface
EAC1 was prepared as described above. Human C4 was incubated with purified DENV NS1 or C4BP for 1 h on ice before adding EAC1. After a 15-min incubation at 30°C, EAC14b were sequentially incubated with C2 and C3 as described above. The deposition of C3b and C4b was determined by staining with anti-C3c and anti-C4c mAbs, respectively. After three washes, cells were incubated with Alexa Fluor 647–conjugated anti–mouse IgG and analyzed by flow cytometry.
Complement activation on the surface of CHO cells
This assay was modified from the published protocols (Barilla-LaBarca et al., 2002; Liszewski et al., 2008) and performed in 96-well plates seeded with 106 cells/well. CHO cells were sensitized with 50 µg/ml rabbit anti-CHO surface antigen IgG at 4°C on a shaker (600 rpm). After a 30 min incubation, the cells were incubated with the mixture of DENV NS1 or BSA (25 µg/ml) and purified human CP complement component C1 (2.5 µg/ml), C2 (2 µg/ml), C3 (10 µg/ml), and C4 (6.67 µg/ml) in GVB2+ buffer for 45 min at 4°C on a shaker. Deposition of C3d and C4d was detected by flow cytometry as described above with a murine mAb to human C3d or C4d (10 µg/ml; Quidel).
Assessment of C4 cleavage
Western blot.
C4 was incubated with NS1 on ice for 1 h. In some experiments, purified C1qrs or C1s was added to an NS1-C4 mixture. At various time points, reducing sample buffer was added, and samples were separated by 10% SDS-PAGE. Western blot was performed using goat anti–human C4 Ab as described above.
C4a ELISA.
Purified C4 was incubated with purified NS1 in the presence or absence of C1-INH (40 µg/ml) on ice for 1 h. After a second 1 h incubation at 37°C, C4a was measured with the BD OptEIA Human C4a ELISA kit (BD).
Direct interaction of NS1 and C1s
Size exclusion chromatography.
Purified WNV NS1 (50 µg) or human proC1s (15 µg) or Fab fragment of murine mAb to WNV E protein (E9-Fab; 15 µg) in PBS was fractionated in a Superose 6 column (GE Healthcare) at a rate of 0.5 ml/min. 15 fractions (1 ml each) were collected and concentrated 10-fold by 0.5 ml centrifugal filter devices (Amicon Ultra; Millipore) before SDS-PAGE and Western blot with biotinylated anti-WNV NS1 mAb 3NS1 (0.5 µg/ml; Chung et al., 2006b) followed by HRP-conjugated streptavidin (1:5,000; Vector Laboratories) or goat antiserum to human C1s (1:5,000; Quidel) followed by donkey anti–goat IgG (1:5,000; Sigma-Aldrich), and HRP-conjugated goat anti–mouse IgG (Sigma-Aldrich; 1:5,000). In some experiments, WNV NS1 was preincubated with proC1s or E9-Fab for 1 h on ice before loading onto a size exclusion column.
ELISA.
Microtiter plates were coated with purified human C1s or proC1s or BSA (10 µg/ml in PBS). After five washes with PBS, nonspecific binding sites were blocked with 2% heat inactivated BSA in PBS for 2 h at room temperature followed by five washes with PBS. Purified WNV, DENV, or YFV NS1 at various concentrations was added to each well and incubated for 2 h at room temperature. Bound WNV or DENV NS1 was detected as described above. A 1:700 dilution of ascites fluid containing the YFV specific anti-NS1 mAb 4E3 (Schlesinger et al., 1985) was used to detect YFV NS1.
Serum neutralization of DENV
Neutralization of DENV by C4-deficient GPS, with and without reconstitution with human C4 and in the presence or absence of DENV NS1 protein, was tested in a plaque assay using BHK-21 cells. Human C4 was incubated with soluble DENV NS1 or BSA (final protein concentration of 50 µg/ml, diluted in gelatin veronal buffer with Mg2+ and Ca2+ [GVB2+]; CompTech) for 1 h at room temperature. DENV2 strain 16681 (2 × 102 PFU) was then added to the mixture of NS1-C4 or BSA-C4, followed by C4-deficient GPS, either untreated or heat inactivated (56°C for 30 min) diluted in GVB2+ buffer to a final serum concentration of 10%. Samples were incubated for 1 h at 37°C and then added to BHK-21 monolayers in duplicate. Infection of BHK-21 cells occurred for 90 min at 37°C; after that the cells were washed extensively with DMEM, overlaid with 1% agarose in Minimal Essential Media supplemented with 2% FBS, and cultured for five days at 37°C. After formaldehyde fixation (10% vol/vol) and staining of wells with a 1% (wt/vol) crystal violet solution in 20% ethanol, plaques were counted.
Statistical analysis
Datasets were compared by a two-tailed, unpaired Student’s t test. Multiple comparisons were performed using an analysis of variance test. Statistical significance was achieved when P values were <0.05.
Online supplemental material
Using preclearance experiments, Fig. S1 shows that the inhibitory activity against C4 in a hemolysis assay is NS1-dependent. Fig. S2 demonstrates that NS1 lacks the ability to regulate C3 convertase or C3 and C5 decay accelerating activity. Fig. S3 shows that NS1 lacks cofactor activity for factor I to degrade C4b. Fig. S4 establishes that the ability of NS1 to promote C4 degradation is specific as proteolysis of C3 was not observed. Fig. S5 provides an analysis of WNV NS1 by SDS-PAGE and Western blot after purification by immunoaffinity and ion-exchange chromatography. Fig. S6 presents an analysis of WNV NS1 by SDS-PAGE and Western blot after purification by size exclusion chromatography.
Acknowledgments
We thank D. Spitzer, S. Schaecher, E. Mehlhop, N. Punyadee, S. Thiemmeca, K. Liszewski, C. Nelson, and D. Fremont for experimental help and advice, R. Kuhn for BHK-YFV-Rep cells, C. Puttikhunt and W. Kasinrerk for providing DENV NS1 specific mAbs, W. Klimstra and D. Lenschow for the Sindbis expression vectors, and J. Schlesinger for YFV NS1 specific mAbs.
This work was supported by the Midwest Regional Centers for Excellence for Biodefense and Emerging Infectious Disease Research (U54-AI057160 to J.P. Atkinson and M.S. Diamond), the Pediatric Dengue Vaccine Initiative (M.S. Diamond), and the National Center for Genetic Engineering and Biotechnology (BIOTEC), Thailand (P. Avirutnan). P. Avirutnan has been supported by a National Institutes of Health postdoctoral training grant from the Division of Dermatology of the Department of Medicine, Washington University School of Medicine, and the Chalermprakeit grant from the Faculty of Medicine Siriraj Hospital, Mahidol University. P. Somnuke is supported by a M.D., PhD training fellowship from Mahidol University.
The authors declare no competing interests.
References
- Ab
antibody
- BHK
baby hamster kidney
- CHO
Chinese hamster ovasry
- CP
classical pathway
- DENV
dengue virus
- DF
dengue fever
- DHF/DSS
dengue hemorrhagic fever/dengue shock syndrome
- E
sheep erythrocytes
- EA
Ab-sensitized E
- fH
factor H
- GPS
guinea pig serum
- HRP
horseradish peroxidase
- MCP
membrane cofactor protein
- MFI
mean fluorescence intensity
- sCR1
soluble complement receptor 1
- WNV
West Nile virus
- YFV
yellow fever virus
Author notes
J.P. Atkinson and M.S. Diamond contributed equally to this paper.