Hematopoietic cell transplantation (HCT) offers curative potential for inborn errors of immunity (IEI) patients, who often enter HCT with significant comorbidities and disease sequelae, active infections, and/or limited donor options. Strategies to enhance engraftment must be balanced against graft-versus-host disease (GVHD) risk and the need for prompt immune reconstitution.
Recipients of T cell-replete HLA-matched (related or unrelated) or HLA-haploidentical grafts (n = 44) received serotherapy-free, radiation-free reduced-intensity conditioning (pentostatin/cyclophosphamide/2 days busulfan), with PTCy, sirolimus, plus/minus mycophenolate mofetil (MMF) as GVHD prophylaxis. Given promising outcomes with very low GVHD incidence in 20 patients who received MMF on post-HCT days 5–35 (MMF35) (1), MMF duration was reduced (MMF18) and/or omitted (MMF0) via a duration de-escalation schema for the subsequent 24 patients (supplemental table).
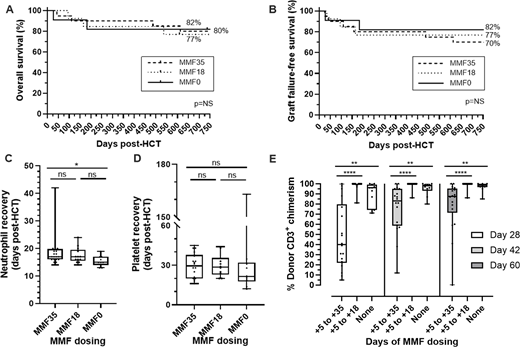
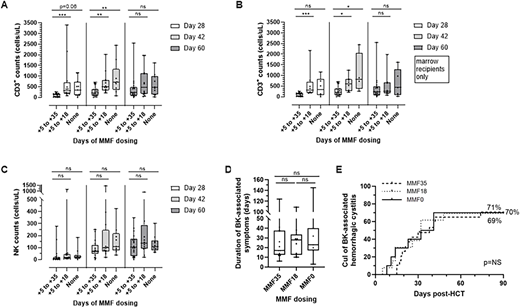
Overall and graft-failure-free survival, along with engraftment kinetics, were largely unaffected by MMF duration, but patients who received MMF18 or MMF0 attained full donor T cell chimerism earlier (Figure 1) and required fewer unplanned donor cell infusions. Lymphocyte reconstitution differed in the T cell, but not natural killer (NK) cell, compartment at days 28 and 42, with higher T cell counts in the MMF18 and MMF0 groups even accounting for graft type, but the effect disappeared by day 60 (Figure 2). Viral complications, including BK-associated cystitis incidence and duration, were similar across cohorts (supplemental table, Figure 2).
Engraftment and survival by mycophenolate mofetil (MMF) exposure. Overall survival (A), graft failure-free survival (B), neutrophil recovery (defined as >500 neutrophils/uL on 3 consecutive days post-HCT) (C), and platelet recovery (defined as >20,000 platelets/uL on 3 consecutive days post-HCT without transfusion in preceding 7 days) (D) do not vary with MMF exposure, except for neutrophil recovery, where the effect disappeared when only marrow grafts were analyzed. Donor CD3+ chimerism at days 28, 42, and 60 is significantly higher in patients with reduced MMF exposure, even accounting for graft type (E). Statistical significance depicted as: ns (p > 0.05), *, (p < 0.05), ** (p < 0.001), *** (p < 0.001), and **** (p < 0.0001).
Engraftment and survival by mycophenolate mofetil (MMF) exposure. Overall survival (A), graft failure-free survival (B), neutrophil recovery (defined as >500 neutrophils/uL on 3 consecutive days post-HCT) (C), and platelet recovery (defined as >20,000 platelets/uL on 3 consecutive days post-HCT without transfusion in preceding 7 days) (D) do not vary with MMF exposure, except for neutrophil recovery, where the effect disappeared when only marrow grafts were analyzed. Donor CD3+ chimerism at days 28, 42, and 60 is significantly higher in patients with reduced MMF exposure, even accounting for graft type (E). Statistical significance depicted as: ns (p > 0.05), *, (p < 0.05), ** (p < 0.001), *** (p < 0.001), and **** (p < 0.0001).
Lymphocyte reconstitution and viral complications by mycophenolate mofetil (MMF) exposure. CD3+ counts are significantly greater at days 28 and 42, but not day 60, post-HCT with reduced MMF exposure (A), and this trend persists if peripheral blood stem cell recipients are excluded (B). NK counts do not vary with MMF exposure (C). Duration of BK-associated symptoms (D) and cumulative incidence (Cul) of BK-associated hemorrhagic cystitis (E) do not vary with MMF exposure. Statistical significance depicted as: ns for p > 0.05, *, p < 0.05, ** for p < 0.01, *** for p < 0.001, and **** for p > 0.0001.
Lymphocyte reconstitution and viral complications by mycophenolate mofetil (MMF) exposure. CD3+ counts are significantly greater at days 28 and 42, but not day 60, post-HCT with reduced MMF exposure (A), and this trend persists if peripheral blood stem cell recipients are excluded (B). NK counts do not vary with MMF exposure (C). Duration of BK-associated symptoms (D) and cumulative incidence (Cul) of BK-associated hemorrhagic cystitis (E) do not vary with MMF exposure. Statistical significance depicted as: ns for p > 0.05, *, p < 0.05, ** for p < 0.01, *** for p < 0.001, and **** for p > 0.0001.
Importantly, there was only 1 infection-related death in the MMF18 and MMF0 cohorts (4%), as compared to 3 in the MMF35 cohort (15%). Among 7 haploidentical HCTs using MMF18, 1 patient experienced engraftment syndrome, later dying of chemotherapy-associated lung toxicity, while another died of GVHD complications and idiopathic pneumonia syndrome; both had received peripheral blood stem cell (PBSC) grafts.
Overall, steroid-refractory acute GVHD occurred only in 2 recipients, both with haploidentical HCTs at MMF18, compared to none in the original MMF35 cohort. Of note, chronic GVHD, mostly mild, occurred only in PBSC recipients.
Reduced MMF duration/omission in our platform is associated with excellent outcomes for matched HCTs. Mismatched HCT outcomes and the role of PBSC vs. marrow graft receipt require further study with larger patient numbers. Across patients, reducing MMF exposure is associated with earlier donor T cell reconstitution and no adverse effect on survival or engraftment.