Chronic spontaneous urticaria (CSU) is a clinical diagnosis managed according to American Academy of Allergy, Asthma & Immunology (AAAAI) and the American College of Allergy, Asthma & Immunology (ACAAI) guidelines, which recommend high-dose second-generation antihistamines as first-line therapy, followed by biologics such as omalizumab, dupilumab, and, more recently, remibrutinib for refractory disease.
When patients fail standard and advanced therapies or develop systemic features, the differential diagnosis should expand to include autoimmune and autoinflammatory disorders. We present a case of refractory chronic urticaria with angioedema in which failure of multiple therapies and subsequent response to anakinra suggest an autoinflammatory component.
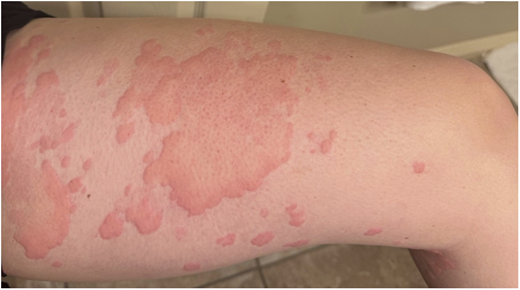
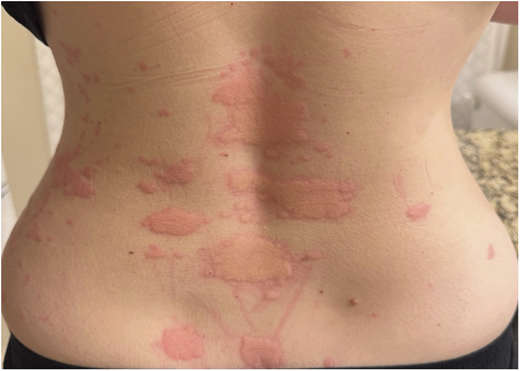
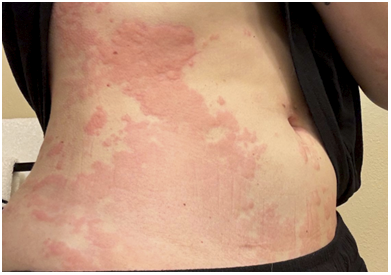
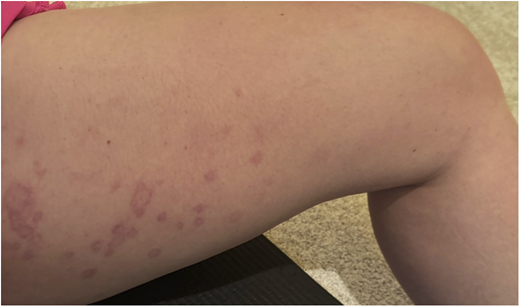
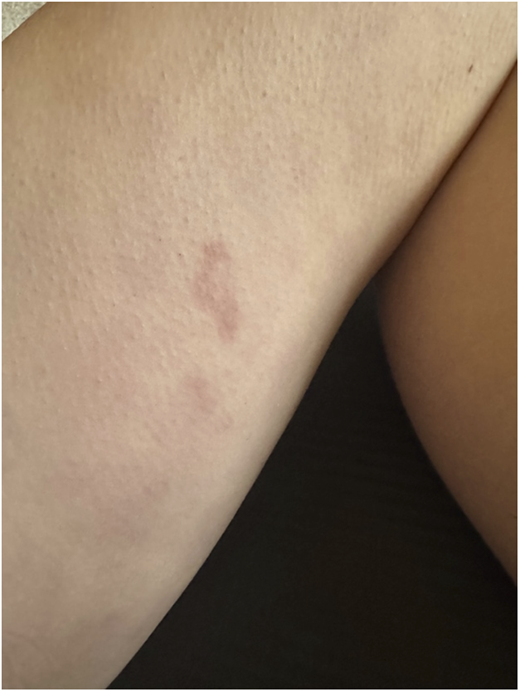
A 34-year-old woman with no significant past medical history presented with a three-month history of recurrent urticaria (Figures 1–3). Initial treatment with high-dose antihistamines, H2 blockers, leukotriene antagonists, and systemic corticosteroids provided only transient relief. Omalizumab was initiated with minimal response, and cyclosporine was added for steroid-dependent disease, but discontinued due to alopecia. Skin biopsy demonstrated a superficial and interstitial dermal infiltrate predominantly composed of neutrophils, with scattered eosinophils and lymphocytes, and no evidence of vasculitis; direct immunofluorescence was normal. Laboratory evaluation, including complete blood count (CBC), erythrocyte sedimentation rate (ESR)/C-reactive protein (CRP), tryptase, and serum protein electrophoresis, was unremarkable. A chronic urticaria index of 18.8 supported type IIb chronic spontaneous urticaria (CSU). Given the neutrophilic predominance on biopsy, dapsone and colchicine were trialed without improvement. The patient continued to experience severe flares requiring recurrent high-dose corticosteroids, resulting in steroid-induced metabolic syndrome requiring treatment with a GLP-1 receptor agonist. Additional therapies, including hydroxychloroquine, tacrolimus, and dupilumab, were ineffective. Lesions were annular and resolved with post-inflammatory hyperpigmentation (Figures 4 and 5).
Urticaria affecting the leg, upper and lower back, and abdomen, shown in Figures 1–3, respectively.
Urticaria affecting the leg, upper and lower back, and abdomen, shown in Figures 1–3, respectively.
Postinflammatory hyperpigmentation affecting the thighs and legs.
Based on histopathologic features and clinical refractoriness, daily anakinra was initiated, leading to marked improvement with near-complete resolution of urticaria and angioedema, though low-dose alternate-day prednisone remained necessary. Subsequent initiation of remibrutinib allowed for complete discontinuation of systemic corticosteroids. Informed consent for publication was obtained from the patient.
This case highlights the heterogeneity underlying chronic urticaria. Neutrophil-predominant infiltrates, steroid dependence, and response to IL-1 blockade suggest an autoinflammatory mechanism rather than classic CSU.
In patients with refractory urticaria, neutrophilic histopathology, and systemic features, clinicians should consider autoinflammatory syndromes and neutrophilic urticarial dermatoses, for which IL-1–targeted therapies may be more effective than standard CSU treatments.