Interleukin (IL)-4 and -13 are related cytokines sharing functional receptors. IL-4 signals through the type I (IL-4Rα/common γ-chain [γc]) and the type II (IL-4Rα/-13Rα1) IL-4 receptors, whereas IL-13 utilizes only the type II receptor. In this study, we show that mouse bone marrow–derived macrophages and human and mouse monocytes showed a much greater sensitivity to IL-4 than to IL-13. Lack of functional γc made these cells poorly responsive to IL-4, while retaining full responsiveness to IL-13. In mouse peritoneal macrophages, IL-4 potency exceeds that of IL-13, but lack of γc had only a modest effect on IL-4 signaling. In contrast, IL-13 stimulated greater responses than IL-4 in fibroblasts. Using levels of receptor chain expression and known binding affinities, we modeled the assemblage of functional type I and II receptor complexes. The differential expression of IL-4Rα, IL-13Rα1, and γc accounted for the distinct IL-4–IL-13 sensitivities of the various cell types. These findings provide an explanation for IL-13's principal function as an “effector” cytokine and IL-4's principal role as an “immunoregulatory” cytokine.
IL-4 and -13 are related cytokines, encoded by closely linked genes (1). IL-4 can signal through either the type I (IL-4Rα/γc) or the type II (IL-4Rα/-13Rα1) IL-4 receptor, whereas IL-13 signals exclusively via the type II IL-4 receptor (2). IL-4 binds to IL-4Rα with high affinity, triggering receptor heterodimerization either with γc or with IL-13Rα1. Downstream intracellular signaling from the IL-4–IL-4Rα–γc complex involves activation of the Jak1 and Jak3 kinases, phosphorylation of the Stat6 transcription factor, and activation of the insulin receptor substrate (IRS)-2– and Dok2-signaling intermediates (3). IL-13 initially binds to IL-13Rα1 with intermediate affinity, and then heterodimerizes with IL-4Rα. The IL-13–IL-13Rα1–IL-4Rα complex activates the Tyk2, Jak2, and Jak1 kinases and Stat6 (2, 4, 5). IL-13 can also bind with high affinity to IL-13Rα2, which is generally regarded to act as a decoy receptor, inhibiting IL-13 binding to IL-13Rα1, and thus the formation of the functional type II receptor complex (6), although it has been reported that the IL-13Rα2 can transduce signals under certain conditions (7). Because γc expression is mainly restricted to hematopoietic cells, in nonhematopoietic cells both IL-4 and -13 are believed to use the type II receptor exclusively. However, it was recently discovered that fibroblasts from IL-13Rα1−/− mice are responsive to IL-4; these cells expressed γc mRNA, suggesting that low levels of type I IL-4 receptor may be expressed in some types of fibroblasts (8).
Despite the many similarities of IL-4 and -13, their principal functions are quite different. In the mouse, priming for Th2 differentiation and immunoglobulin class switching are exclusive properties of IL-4, presumably because mouse T and B cells, lacking IL-13Rα1, express type I but not type II receptors. In contrast, many effector functions, including airway hypersensitivity and mucus metaplasia in response to challenge with an antigen to which T cells have been sensitized, can be blocked by anti–IL-13, but not by anti–IL-4 (9–11), indicating that IL-13 is the dominant effector cytokine. Thus, it can be argued that IL-4 acts mainly as a regulatory cytokine and IL-13 largely as an effector cytokine.
Macrophages are among the few cell types that express both type I and II receptors. They are involved in both innate and adaptive immune responses by expressing cytokines, by functioning as antigen-presenting cells, and by phagocytosing antigen-bearing entities. M-CSF induces macrophage differentiation from BM myeloid stem cells into blood monocytes, and subsequently into tissue macrophages (12). In peripheral tissues, tight control of macrophage activation and deactivation is crucial for maintenance of homeostasis. Classical macrophage activation during Th1 responses by IFN-γ and LPS is well characterized, but recently, macrophage activation by IL-4 and -13 has been studied in detail (13, 14). This type II (also termed “alternative”) macrophage activation by IL-4 and -13 is essential for clearance of Schistosoma mansoni infection because mice lacking IL-4Rα expression in macrophages succumb to this helminth (15). In the mouse, type II macrophage activation induces expression of genes that are important for granuloma formation (16) or digesting chitin, which is widely expressed on yeast, arthropods, and nematodes (17, 18).
Here, we studied the effects of IL-4 and -13 on various monocyte/macrophage populations. We show that BM-derived macrophages (BMDMs), as well as human and mouse monocytes, are far more sensitive to IL-4 than to IL-13. The heightened IL-4 sensitivity of these cell types is totally dependent on the type I IL-4 receptor because the lack of functional γc renders the cells less responsive to IL-4 than to IL-13. Like BMDMs, resident peritoneal macrophages (PMs) from WT mice are more sensitive to IL-4 than to IL-13, but show relatively modest changes in their response to IL-4 in the absence of γc. Thus, these two macrophage cell types, when expressing only the type II receptor, nonetheless differ in their relative sensitivity to IL-4 and -13. We show that this difference can be explained by differential expression of IL-13Rα1 between BMDMs and PMs and by the differences in affinity of IL-4 and -13 for the components of their receptors. Among human monocytes, those with an “inflammatory” precursor phenotype (CD14hi, CD16lo) appear more like peritoneal mouse macrophages, whereas monocytes with a “resident” phenotype (CD14lo, CD16hi) are more similar to BMDMs. Finally, in nonhematopoietic cells, namely fibroblasts and epithelial cells, IL-13 stimulates equal or greater responses than does IL-4. The differential responsiveness of these various cell types, based on their differential expression of IL-4–IL-13 receptor chains, helps to explain the distinct function of the two cytokines.
Results
Mouse BMDMs have increased sensitivity to IL-4 over -13
M-CSF–induced in vitro differentiation of BM cells is a well-characterized and widely used method to obtain large numbers of macrophages. Because BMDMs are not subjected to proinflammatory cytokines or Toll-like receptor (TLR) ligands during in vitro differentiation, we hypothesized they would represent an immature or naive population of macrophages, possibly analogous to monocytes. To study IL-4– and IL-13–induced responses in BMDMs, we chose to investigate the activation of Stat6, a key transcription factor activated by these cytokines. An indispensable event in Stat6 activation upon cytokine stimulation is the phosphorylation of tyrosine residue 641 (19). BMDMs showed markedly greater sensitivity to IL-4 than to IL-13 in the induction of phosphorylation of Y641 of Stat6, as detected by flow cytometry (Fig. 1 A, top). BMDMs responded to 0.1 ng/ml of IL-4, and 1 ng/ml of IL-4 caused close to maximal Stat6 Y641 phosphorylation, whereas 10 ng/ml of IL-13 was required to obtain detectable phosphorylation and 100 ng/ml to match the phosphorylation induced by 1 ng/ml of IL-4. The relative difference of IL-4– and IL-13–induced Stat6 Y641 phosphorylation in BMDMs that we measured by intracellular flow cytometry was verified by immunoblotting (Fig. S1).
The greater sensitivity of BMDMs to IL-4 compared with IL-13 requires the type I IL-4 receptor. (A) BMDMs were prepared from three to five individual WT (top) or γc−/− (bottom) mice. The cells were stimulated with IL-4 or -13, as indicated, for 15 min or left unstimulated. The cells were stained with anti-PY641Stat6 and analyzed by flow cytometry. Results shown here are from a representative of five independent experiments. (B) The difference in MFI of stimulated versus nonstimulated cells from both WT and γc−/− BMDMs from five independent experiments; means and SEMs for results from the distinct experiments are shown. (C) Stat6 DNA binding in WT and γc−/− BMDMs. The cells were stimulated as indicated, and nuclear lysates were prepared and analyzed by EMSA with a radioactively labeled DNA probe (SBE1) that contains a Stat6 binding site. (D) IL-4 binding to γc−/− BMDMs is not impaired. WT and γc−/− BMDMs, prepared as described in A, were incubated with or without IL-4 for 30 min at 4°C, and cells were washed and stained with anti–IL-4Rα (M1), followed by flow cytometry; MFI of M1 binding is indicated. Results shown are from one of two replicate experiments. (E) IL-4–induced Stat6 DNA binding is undetectable in Jak3−/− BMDMs. BMDMs from a Jak3-deficient mouse were stimulated as indicated and subjected to EMSA assay as in C.
The greater sensitivity of BMDMs to IL-4 compared with IL-13 requires the type I IL-4 receptor. (A) BMDMs were prepared from three to five individual WT (top) or γc−/− (bottom) mice. The cells were stimulated with IL-4 or -13, as indicated, for 15 min or left unstimulated. The cells were stained with anti-PY641Stat6 and analyzed by flow cytometry. Results shown here are from a representative of five independent experiments. (B) The difference in MFI of stimulated versus nonstimulated cells from both WT and γc−/− BMDMs from five independent experiments; means and SEMs for results from the distinct experiments are shown. (C) Stat6 DNA binding in WT and γc−/− BMDMs. The cells were stimulated as indicated, and nuclear lysates were prepared and analyzed by EMSA with a radioactively labeled DNA probe (SBE1) that contains a Stat6 binding site. (D) IL-4 binding to γc−/− BMDMs is not impaired. WT and γc−/− BMDMs, prepared as described in A, were incubated with or without IL-4 for 30 min at 4°C, and cells were washed and stained with anti–IL-4Rα (M1), followed by flow cytometry; MFI of M1 binding is indicated. Results shown are from one of two replicate experiments. (E) IL-4–induced Stat6 DNA binding is undetectable in Jak3−/− BMDMs. BMDMs from a Jak3-deficient mouse were stimulated as indicated and subjected to EMSA assay as in C.
To better understand how the type II IL-4 receptor transduces IL-4 signals in BMDMs, we used γc−/− mice as a source for these cells because these cells are unable to form type I IL-4 receptor complexes. BMDMs derived from WT or γc−/− animals were similar in numbers generated and in phenotype (20). Approximately 95% of both WT and γc−/− BMDMs were CD11b+ and F4/80+ (unpublished data). However, in γc−/− BMDMs, Y641 phosphorylation of Stat6 was first detected at 10 ng of IL-4/ml, and there was no greater phosphorylation at 100 or 200 ng/ml (Fig. 1 A, bottom, and not depicted). IL-13–induced Stat6 phosphorylation was equivalent in γc−/− and WT BMDMs. In γc−/− BMDMs, 10 ng/ml of IL-13 induced Stat6 phosphorylation to the same extent as IL-4 at 10 ng/ml, and it exceeded that induced by IL-4 at 100 and 200 ng/ml. The difference of Stat6 phosphorylation in response to cytokine stimulation in WT and γc−/− cells was quantified by subtracting the median fluorescence intensity (MFI) of the unstimulated sample from the MFI of the stimulated sample (Fig. 1 B). Fig. 1 B shows results from five independent experiments. Furthermore, DNA-binding of Stat6 as measured by electrophoretic mobility shift assay (EMSA) was virtually absent in γc−/− BMDMs stimulated with IL-4 at concentrations ranging from 0.1 to 10 ng/ml, whereas the DNA-binding response to IL-13 at 10 ng/ml was unimpaired in γc−/− BMDMs (Fig. 1 C). Defective IL-4–induced signaling in γc−/− BMDMs was not caused by an inability of IL-4 to bind IL-4Rα because IL-4 blocked the capacity of anti–IL-4Rα to bind to IL-4Rα equally in WT and γc−/− BMDMs. (Fig. 1 D).
Jak3 is associated with γc, and is critical in mediating signals from the type I, but not the type II, IL-4 receptor (21). BMDMs were prepared from Jak3−/− mice. As shown in Fig. 1 E, IL-4–induced Stat6 DNA binding is undetectable in Jak3−/− cells at 10 ng/ml, whereas IL-13–elicited Stat6 DNA binding is intact in Jak3−/− BMDMs. Thus, these results further emphasize that BMDM responses to IL-4 are highly dependent on the type I receptor. As expected, IFN-γ has no effect on Stat6 DNA-binding activity in either WT or Jak3−/− cells.
IL-4– and IL-13–mediated gene induction in BMDMs
Type II macrophage activation results in induction of several genes, including arginase (Arg) 1. Arg1 plays an important role in regulating macrophage responses, as Arg1 decreases nitric oxide synthase production, and thus nitric oxide, by consuming the substrate, cellular l-arginine (22). The promoter of Arg1 contains a Stat6 binding site (23), and Arg1 mRNA is induced in mouse macrophages by IL-4 (24). As shown in Fig. 2 A, Arg1 mRNA induction at 2 h could be detected in response to 1 ng/ml of IL-4, and peaked at 10 ng/ml (mean of fold induction, 247). In contrast, IL-13 at <10 ng/ml did not induce detectable Arg1, and its peak induction (mean of fold induction, 79) was only ∼30% of the levels induced by IL-4 (Fig. 2 A). In γc−/− BMDMs, IL-13 induction of Arg1 was comparable to that observed in WT BMDMs, but IL-4 induction of Arg1 was virtually undetectable, even at 100 ng/ml (Fig. 2 A). Anti–IL-4Rα (M1) inhibited IL-13-induced Arg1 expression in both WT and γc−/− BMDMs, confirming that IL-13 responses require the IL-4 receptor-α chain (Fig. 2 C) and that the IL-13 response could not be attributed to a non–IL-4Rα–using receptor. The importance of Stat6 in the response to both IL-4 and -13 was demonstrated by the failure of both cytokines to induce Arg1 expression, even at 100 ng/ml in Stat6−/− BMDMs (Fig. 2 B).
IL-4–induced Arg1 expression in BMDMs is dependent on the type I IL-4 receptor and Stat6 expression. (A) BMDMs from WT and γc−/− mice prepared as in Fig. 1 A were unstimulated or stimulated with indicated concentrations of IL-4 or -13 for 2 h. Cells were lysed, RNA was purified and transcribed to cDNA, and RT-PCR performed to measure Arg1 expression. The results were normalized to 18S RNA. The experiment was performed independently three times; means and SEMs of results from the individual experiments are shown. (B) BMDMs were prepared from Stat6-deficient B6 mouse and left untreated or treated with indicated concentrations of IL-4 or IL-13. Thereafter, the experiment was performed as in A. The experiment was performed independently three times; means and SEMs of results from the individual experiments are shown. (C) BMDMs from WT and γc−/− mice treated for 1 h at 37°C with blocking antibody against IL-4Rα (M1) as indicated, followed by stimulation with IL-4 or -13 (10 and 200 ng/ml, respectively) for 2 h. Cells were lysed and Arg1 mRNA induction measured as in A.
IL-4–induced Arg1 expression in BMDMs is dependent on the type I IL-4 receptor and Stat6 expression. (A) BMDMs from WT and γc−/− mice prepared as in Fig. 1 A were unstimulated or stimulated with indicated concentrations of IL-4 or -13 for 2 h. Cells were lysed, RNA was purified and transcribed to cDNA, and RT-PCR performed to measure Arg1 expression. The results were normalized to 18S RNA. The experiment was performed independently three times; means and SEMs of results from the individual experiments are shown. (B) BMDMs were prepared from Stat6-deficient B6 mouse and left untreated or treated with indicated concentrations of IL-4 or IL-13. Thereafter, the experiment was performed as in A. The experiment was performed independently three times; means and SEMs of results from the individual experiments are shown. (C) BMDMs from WT and γc−/− mice treated for 1 h at 37°C with blocking antibody against IL-4Rα (M1) as indicated, followed by stimulation with IL-4 or -13 (10 and 200 ng/ml, respectively) for 2 h. Cells were lysed and Arg1 mRNA induction measured as in A.
IL-4– and IL-13–induced responses in PMs and NIH3T3 fibroblasts
We next compared IL-4– and IL-13–induced Stat6 phosphorylation in tissue macrophages. We initially examined resident PMs obtained from mouse peritoneal lavages. Typically, these cells were 80–90% positive for both CD11b and F4/80. These cells were even more sensitive than BMDMs to IL-4. IL-4–induced Stat6 Y641 phosphorylation was nearly maximal at 0.1 ng/ml (Fig. 3 A, top) and, at this concentration of IL-4, the P value for the comparison of the degree of Stat6 phosphorylation between BMDMs and PMs, by the unpaired Student's t test, was statistically significant (0.014). In contrast to BMDMs, where IL-13 induced no Stat6 phosphorylation at concentrations <10 ng/ml, IL-13 induced substantial Stat6 phosphorylation in PMs at 1 ng/ml, and was close to the IL-4 maximum at 10 ng/ml. The P value for the comparison of the degree of Stat6 phosphorylation between BMDMs and PMs at 10 ng of IL-13 by unpaired Student's t test was statistically significant (0.020). In striking contrast to γc−/− BMDMs, PMs from γc−/− donors showed only a modest reduction in their sensitivity to IL-4 and were clearly more sensitive to IL-4 than to IL-13 (Fig. 3 A, bottom). The P values for the comparison of the degree of Stat6 phosphorylation between γc−/− BMDMs and PMs at concentrations of IL-4 at or >1 ng/ml are statistically significant (1 ng/ml, 0.003; 10 ng/ml, 0.046; 100 ng/ml, 0.0003). Thus, in PMs, IL-4 efficiently uses the type II receptor, which it does not in BMDMs, and IL-13 is a relatively better stimulant in PMs than in BMDMs. The data are quantitated in Fig. 3 B, similar to the data in Fig. 1 B, and represents five experiments for the wild-type cells and three for the γc−/− cells. Collectively, IL-4 appears to be an ∼100-fold more potent inducer of Stat6 Y641 phosphorylation than IL-13 in both WT BMDMs and PMs, but a deficiency of functional type I IL-4 receptors has a fundamentally different impact on IL-4 responsiveness in these two macrophage populations.
PMs are highly sensitive to IL-4, but IL-4 responses are not exclusively dependent on type IL-4 receptor. (A) PMs were purified from three to five WT (top) and γc−/− (bottom) mice by adhesion after peritoneal lavage. The cells were rested for 2 d in media containing 2% FBS, and then stimulated for 15 min with IL-4 or -13 or left unstimulated and analyzed as in Fig. 1 A. Results of representative experiments are shown. (B) The difference of MFI of stimulated versus nonstimulated cells from both WT and γc−/− PMs in A was quantitated; means and SEMs from independent experiments are shown. For WT cells, the experiment was performed five times; for γc−/− cells, three times. (C) PMs were prepared from WT and γc−/− as described. The cells were stimulated as indicated for 2 h or left unstimulated. Thereafter, Arg1 mRNA induction was measured as in Fig. 2 A. The experiment was performed three times; means and SEMs of results from independent experiments are shown. (D) Tg was injected i.p. into 5 mice; 3 d later, they were killed, and PMs were purified and analyzed as in A. The experiment was performed twice with similar results. (E) NIH3T3 fibroblasts were starved in growth media containing 1% FBS overnight. Subsequently, the cells were either left unstimulated or stimulated with IL-4 or -13 as indicated for 15 min. To study Stat6 Y641 phosphorylation, the cells were permeabilized, stained, and analyzed as in Fig. 1 A. Means and SEMs of results from four independent experiments are shown.
PMs are highly sensitive to IL-4, but IL-4 responses are not exclusively dependent on type IL-4 receptor. (A) PMs were purified from three to five WT (top) and γc−/− (bottom) mice by adhesion after peritoneal lavage. The cells were rested for 2 d in media containing 2% FBS, and then stimulated for 15 min with IL-4 or -13 or left unstimulated and analyzed as in Fig. 1 A. Results of representative experiments are shown. (B) The difference of MFI of stimulated versus nonstimulated cells from both WT and γc−/− PMs in A was quantitated; means and SEMs from independent experiments are shown. For WT cells, the experiment was performed five times; for γc−/− cells, three times. (C) PMs were prepared from WT and γc−/− as described. The cells were stimulated as indicated for 2 h or left unstimulated. Thereafter, Arg1 mRNA induction was measured as in Fig. 2 A. The experiment was performed three times; means and SEMs of results from independent experiments are shown. (D) Tg was injected i.p. into 5 mice; 3 d later, they were killed, and PMs were purified and analyzed as in A. The experiment was performed twice with similar results. (E) NIH3T3 fibroblasts were starved in growth media containing 1% FBS overnight. Subsequently, the cells were either left unstimulated or stimulated with IL-4 or -13 as indicated for 15 min. To study Stat6 Y641 phosphorylation, the cells were permeabilized, stained, and analyzed as in Fig. 1 A. Means and SEMs of results from four independent experiments are shown.
In WT PMs, IL-4–induced Arg1 expression was somewhat greater than that induced by IL-13 (Fig. 3 C). In γc−/− PMs, IL-4–induced Arg1 expression was slightly decreased, but in contrast to γc−/− BMDMs, the lack of γc markedly affected Arg1 expression only at the lowest cytokine concentration studied (1 ng/ml; Fig. 3 C).
The responses to IL-4 and -13 by peritoneal exudate macrophages induced by thioglycollate (Tg) were generally similar to those of resident PMs, although their sensitivity to IL-4 was somewhat less than that of PMs, and they displayed only a minimal response to IL-13 at 1 ng/ml, but quite good responses at 10 ng/ml (Fig. 3 D).
We also compared IL-4 and -13 responses in cells that mainly or exclusively express the type II IL-4 receptor. For this purpose, we tested Stat6 phosphorylation in response to IL-4 and -13 in NIH3T3 fibroblasts. Overnight-starved NIH3T3 cells were stimulated for 15 min with increasing concentrations of IL-4 and -13. At concentrations >0.1 ng/ml, IL-13 induced Stat6 Y641 phosphorylation substantially better than IL-4 in fibroblasts (Fig. 3 F). In a human lung epithelial cell line (H292), 20 ng/ml of IL-4 and -13 induced comparable tyrosine phosphorylation of immunoprecipitated Stat6 (Fig. S2).
Mouse monocytes show increased sensitivity to IL-4
Monocytes are macrophage precursors that circulate in blood. They are released into the bloodstream upon differentiation of the common myeloid progenitor cells in BM (25). Because we hypothesized that BMDMs might represent a relatively immature macrophage pool, we wished to determine whether there are differences in IL-4– and IL-13–induced signaling in these macrophage precursors that would be similar to the differences we detected in BMDMs. Mouse blood monocytes from WT B6 mice were analyzed for responsiveness to IL-4 and -13 by measuring Stat6 Y641 phosphorylation by flow cytometry. IL-4 induced substantial responses at 0.1 ng/ml in monocytes, whereas IL-13 required 10 ng/ml to obtain measureable responses (Fig. 4 A). Because of limitations in cell numbers, we did not test responsiveness to 1 ng/ml or 100 ng/ml of either IL-4 or -13. Monocytes from γc−/− mice responded poorly to both IL-4 and -13 at 0.1 ng/ml, and slightly better to IL-13 than to IL-4 at 10 ng/ml (Fig. 4 B). Thus, the IL-4 sensitivity of γc−/− monocytes resembled that of γc−/− BMDMs.
The Type I IL-4 receptor is essential for responses to low concentrations of IL-4 responses in mouse monocytes. (A) Blood leukocytes were obtained from three to four WT B6 mice. After lysing erythrocytes, the cells were rested in 2% FBS containing medium for 2 h, and then stimulated for 15 min with indicated concentrations of IL-4 and -13 or left unstimulated. Subsequently, the cells were stained for CD11b and F4/80, followed by permeabilization and staining for Y641 of Stat6. The Stat6 phosphorylation of CD11b+ and F4/80+ cells was evaluated as in Fig. 1 A. To study the effect of IL-4 and -13 on blood monocytes in γc−/− mice (B), identical experiments were performed in these mice. A representative experiment is illustrated by the flow cytometry plots; the plot of cytokine concentration versus Δ Median represents data from three independent experiments; the mean and SEM of the results from these independent experiments are shown.
The Type I IL-4 receptor is essential for responses to low concentrations of IL-4 responses in mouse monocytes. (A) Blood leukocytes were obtained from three to four WT B6 mice. After lysing erythrocytes, the cells were rested in 2% FBS containing medium for 2 h, and then stimulated for 15 min with indicated concentrations of IL-4 and -13 or left unstimulated. Subsequently, the cells were stained for CD11b and F4/80, followed by permeabilization and staining for Y641 of Stat6. The Stat6 phosphorylation of CD11b+ and F4/80+ cells was evaluated as in Fig. 1 A. To study the effect of IL-4 and -13 on blood monocytes in γc−/− mice (B), identical experiments were performed in these mice. A representative experiment is illustrated by the flow cytometry plots; the plot of cytokine concentration versus Δ Median represents data from three independent experiments; the mean and SEM of the results from these independent experiments are shown.
Human monocyte sensitivity to IL-4 over -13 is dependent on γc and occurs in CD14hi and CD16hi subtypes
Easy accessibility to a large number of monocytes in human peripheral blood and the relatively low number of monocytes in mice, prompted us to examine the IL-4– and IL-13–induced Stat6 activation in human monocytes. IL-4 induced substantial Stat6 Y641 phosphorylation by elutriated human monocytes at concentrations as low as 0.1 ng/ml; maximum Stat6 phosphorylation was obtained at 1–10 ng/ml of IL-4 (Fig. 5 A). In contrast, IL-13 caused no detectable Stat6 phosphorylation at 0.1 ng/ml and detectable phosphorylation at 1 ng/ml; 10 ng/ml of IL-13 induced close to maximal Stat6 phosphorylation. Consistent with the FACS data, IL-13 failed to induce Stat6 DNA binding at concentrations <10 ng/ml, as demonstrated by EMSA (Fig. 5 B), whereas 0.1 ng/ml of IL-4 induced striking Stat6 DNA binding. These results indicate that human monocytes are also 10–100-fold more sensitive to IL-4 than to IL-13.
Human monocytes are more sensitive to IL-4 than to IL-13. (A) Freshly elutriated human monocytes from individual donors were cultured in RPMI containing 2% FBS for 2 h. The cells were left untreated or treated with indicated concentrations of IL-4 or -13 for 15 min. Subsequently, the cells were fixed, permeabilized, and stained with anti-pStat6Y641. Stat6 phosphorylation was measured in the indicated flow cytometry monocyte gate. For each cytokine concentration, MFI of Stat6 phosphorylation was obtained by subtracting the median of the unstimulated sample from the median of the stimulated sample in monocyte gate (bottom). A representative of five independent experiments is illustrated in the flow cytometry plots. The graph relating cytokine concentration to Δ Median represents five independent experiments, with means and SEMs. (B) Elutriated human monocytes were either left unstimulated or were stimulated with the indicated concentrations of cytokines for 30 min at 37°C. Nuclear protein extracts were then prepared, and the levels of Stat6 activity were measured by EMSA using a Stat6 binding site containing radioactively labeled DNA-probe (SBE1). (C) Blocking of γc inhibits IL-4 responses in human monocytes. The experiment was performed as in B, but the cells were pretreated for 1 h with a blocking antibody against human γc. (D) Differential sensitivity of CD16hi and CD14hi monocytes toward IL-4 and -13. Elutriated monocytes were treated as in A. The cells were stained with anti-CD14 and -CD16 surface antibodies, before fixing and permeabilizing the cells. After methanol permeabilization, the cells were stained with anti-pStat6Y641 antibody. Staining results from donor number 4 in E are shown. (E) Summary of results of IL-4– and IL-13–induced Stat6 phosphorylation in CD14hi and CD16hi human monocytes from four donors; means and SEMs are shown. (F) Expression of IL-4Rα, γc, IL-13Rα1, and IL-13Rα2 in CD14hi and CD16hi monocyte populations was measured by flow cytometry. The expression was quantitated by subtracting the MFI of specific staining from the MFI of the isotype control and dividing the obtained value by the MFI of the unstained control. Monocytes from seven healthy donors were analyzed; means and SEMs are shown.
Human monocytes are more sensitive to IL-4 than to IL-13. (A) Freshly elutriated human monocytes from individual donors were cultured in RPMI containing 2% FBS for 2 h. The cells were left untreated or treated with indicated concentrations of IL-4 or -13 for 15 min. Subsequently, the cells were fixed, permeabilized, and stained with anti-pStat6Y641. Stat6 phosphorylation was measured in the indicated flow cytometry monocyte gate. For each cytokine concentration, MFI of Stat6 phosphorylation was obtained by subtracting the median of the unstimulated sample from the median of the stimulated sample in monocyte gate (bottom). A representative of five independent experiments is illustrated in the flow cytometry plots. The graph relating cytokine concentration to Δ Median represents five independent experiments, with means and SEMs. (B) Elutriated human monocytes were either left unstimulated or were stimulated with the indicated concentrations of cytokines for 30 min at 37°C. Nuclear protein extracts were then prepared, and the levels of Stat6 activity were measured by EMSA using a Stat6 binding site containing radioactively labeled DNA-probe (SBE1). (C) Blocking of γc inhibits IL-4 responses in human monocytes. The experiment was performed as in B, but the cells were pretreated for 1 h with a blocking antibody against human γc. (D) Differential sensitivity of CD16hi and CD14hi monocytes toward IL-4 and -13. Elutriated monocytes were treated as in A. The cells were stained with anti-CD14 and -CD16 surface antibodies, before fixing and permeabilizing the cells. After methanol permeabilization, the cells were stained with anti-pStat6Y641 antibody. Staining results from donor number 4 in E are shown. (E) Summary of results of IL-4– and IL-13–induced Stat6 phosphorylation in CD14hi and CD16hi human monocytes from four donors; means and SEMs are shown. (F) Expression of IL-4Rα, γc, IL-13Rα1, and IL-13Rα2 in CD14hi and CD16hi monocyte populations was measured by flow cytometry. The expression was quantitated by subtracting the MFI of specific staining from the MFI of the isotype control and dividing the obtained value by the MFI of the unstained control. Monocytes from seven healthy donors were analyzed; means and SEMs are shown.
Blocking the type I receptor on human monocytes with γc neutralizing antibody had no inhibitory effect on the Stat6 DNA-binding activity induced by IL-13 (Fig. 5 C), but the Stat6 DNA-binding induced by IL-4 was markedly reduced, indicating that type I IL-4 receptors are essential for IL-4 responses in human monocytes, despite the fact that there is sufficient type II receptor to mediate an IL-13 response.
Human peripheral blood monocytes consist of at least two subpopulations, i.e., CD14hi/CD16lo and CD14lo/CD16hi, with ∼75% being CD14hi/CD16lo. There is still some debate as to the roles of these subpopulations in homeostasis, infections, and inflammatory responses (26, 27), but the CD14hi/CD16lo are often considered precursors of inflammatory macrophages, and the CD14lo/CD16hi are considered precursors of resident macrophages. We wished to determine if IL-4– and IL-13–induced responses might be different in these monocyte subsets. To exclude contaminating cells, we stained elutriated human peripheral monocyte preparations with anti-CD3, -CD19, and -CD56 to exclude T-, B-, and NK cells. In the CD16hi-positive gate, we detected very few contaminating cells (CD3, ∼2%; CD19, ∼0%; or CD56, ∼1%), and in the CD14hi population, there was ∼5% CD56+ and ∼3% CD3+ cells, but no detectable CD19-expressing cells (unpublished data). We examined IL-4– and IL-13–induced Stat6 Y641 phosphorylation in these two subsets. Both IL-4 and -13 were able to induce Stat6 activation at lower concentrations in CD14hi/CD16lo than in CD14lo/CD16hi population (Fig. 5 D). To further confirm this observation, we compared the IL-4 and -13 responsiveness of four independent donors with similar results (Fig. 5 E).
Collectively, these results confirm the superiority of IL-4 in inducing Stat6 activation in human monocytes and, further, that this advantage is lost when the type I IL-4 receptor is inhibited. Finally, the CD14hi monocyte subset is more sensitive to both IL-4 and -13 than the CD16hi monocyte subpopulation. The difference between monocyte populations is particularly clear in the response to IL-13 at 10 ng/ml. In that respect, the CD14hi population resembles the PM population and the CD14lo resembles the BMDM population. In accord with these differences in IL-4–IL-13 sensitivity between human monocyte populations, we observed that IL-4Rα, γc, and IL-13Rα1 are more highly expressed in the CD14hi populations, and that IL-13Rα2 is barely expressed in either as measured by flow cytometry (Fig. 5 F).
Receptor chain expression in BMDMs, PMs, and NIH3T3 fibroblasts
Measurements of binding properties of the components of the type I and II receptors and recent structural characterization of type I and II IL-4 receptors (28) suggested that relative receptor chain expression might provide a mechanism to regulate the relative potency of IL-4 and -13. Indeed, the analysis of receptor chain expression in the human monocyte subpopulations supports this idea (Fig. 5 F). We examined the expression of different receptor chains on BMDMs and PMs by flow cytometry, and representative stainings are shown in Fig. 6 A. We quantitated the data from independent stainings in Fig. 6 B. γc expression was detected clearly on both BMDMs and PMs, with fourfold higher expression on PMs. IL-4Rα expression was 2.6-fold higher on PMs than on BMDMs (Fig. 6 B).
Expression of type I and II IL-4 receptor complex chains on BMDMs and PMs. (A) γc and IL-4Rα chain expression in WT and γc−/− BMDMs and PMs. Cells were washed twice and stained for 20 min at 4°C, washed again twice, and subjected to flow cytometric analysis. Representative stainings for each cell type are shown. (B) Quantitated data from the cell surface stainings of 7 (BMDMs) or 5 (PMs) independent experiments are shown. The analysis was performed as in Fig. 5 F. (C) IL-13 receptor expression in BMDMs and PMs. 2 × 105 BMDMs and PMs were lysed, 150 μg of total cell lysate was separated on PAGE gel, followed by Western blotting and immunostaining against IL-13Rα1. Equal loading and transfer was verified with Ponceau S staining.
Expression of type I and II IL-4 receptor complex chains on BMDMs and PMs. (A) γc and IL-4Rα chain expression in WT and γc−/− BMDMs and PMs. Cells were washed twice and stained for 20 min at 4°C, washed again twice, and subjected to flow cytometric analysis. Representative stainings for each cell type are shown. (B) Quantitated data from the cell surface stainings of 7 (BMDMs) or 5 (PMs) independent experiments are shown. The analysis was performed as in Fig. 5 F. (C) IL-13 receptor expression in BMDMs and PMs. 2 × 105 BMDMs and PMs were lysed, 150 μg of total cell lysate was separated on PAGE gel, followed by Western blotting and immunostaining against IL-13Rα1. Equal loading and transfer was verified with Ponceau S staining.
For mouse IL-13Rα1, no suitable monoclonal antibody is available. We failed to detect a reliable specific signal with flow cytometry using a polyclonal anti–IL-13Rα1 antiserum. Therefore, we measured IL-13Rα1 expression by immunoblotting. Using antibody against IL-13Rα1, we observed a stronger ∼50-kD band in extracts from PMs than in extracts from BMDMs; equal loading was confirmed by Ponceau S staining. By densitometry, PMs expressed 2.5-fold more IL-13Rα1 than did BMDMs (Fig. 6 C).
Because fibroblasts from IL-13Rα1−/− mice have recently been reported to respond to IL-4 (8), we examined expression of γc, IL-4Rα, IL-13Rα1, and IL-13Rα2 on NIH3T3 cells. We did not detect IL-13Rα2 mRNA in these cells, and γc mRNA expression was very low (unpublished data). At the protein level, very low levels of γc and IL-4Rα expression were detected by flow cytometry. By immunoblotting, IL-13Rα1 was more highly expressed in fibroblasts than in BMDMs; IL-13Rα2 was undetectable (Fig. S3).
Modeling of functional receptor assemblage in response to IL-4 and -13
Our results thus indicate that monocytes and macrophages are exquisitely sensitive to IL-4 and relatively insensitive to IL-13. Furthermore, the IL-4 response of BMDMs and monocytes from γc−/− donors is severely impaired, indicating strong dependence on the type I receptor, whereas PMs efficiently respond to IL-4 through the type II receptor. Finally, fibroblasts, relying largely or exclusively on the type II receptor, are more sensitive to IL-13 than to IL-4. How are we to understand these differences and, particularly, to explain the capacity of γc−/− PMs to respond better to IL-4 than to IL-13 and for γc−/− BMDMs to respond to IL-13 equally or better than to IL-4, despite the fact that both cell types use only the type II receptor?
To rationalize these observations, one needs to take into account the relative expression of the key receptor chains on the various cells and the equilibrium constants that describe the binding events. Based on our flow cytometric measurements of receptor chain expression, IL-4Rα levels are 2.6-fold higher in PMs than in BMDMs; γc levels are 4 times higher in PMs than BMDMs; and IL-13Rα1 levels are 2.5 times higher in PMs than BMDMs. Neither BMDMs, PMs, nor NIH3T3 have detectable mRNA for IL-13Rα2. Macrophage cell lines have been shown to contain 160–2,300 IL-4Rα, whereas NIH3T3 cells have ∼500 IL-4Rα (29, 30). Human monocytes, which are macrophage precursors and may represent immature macrophage population similar to BMDMs, have been reported to express ∼120 IL-13 binding sites (31), which are presumably IL-13Rα1 (32). For analysis here, we assumed 1,000 IL-4Rα, 1,000 γc, and 200 IL-13Rα1 are expressed by BMDMs. The corresponding levels of expression on PMs would be 2,600, 4,000, and 500, respectively. The equilibrium constants of the binding of the cytokines to their binding chains have been measured, whereas the two-dimensional equilibrium constants of the binding of membrane-associated cytokine/binding chain complex to γc, IL-13Rα1, or IL-4Rα remain as free parameters, but may be estimated from the data available for similar membrane receptors (33) and from the measured solution binding constants (28).
For the purposes of modeling, we have adapted the following values: IL-4 binding to IL-4Rα, kA = 1010 M−1 (34); IL-13 binding to IL-13Rα1, kA = 0.33 × 108 M−1 (35); γc binding to IL-4–IL-4Rα, two dimensional kA = 0.01 μm2 (33); IL-13Rα1 binding to IL-4–IL-4Rα, two dimensional kA = 0.01 μm2 (33); IL-4Rα binding to IL-13/-13Rα1, two dimensional kA = 0. 3 μm2 (33).
The implications of the relative numbers of receptors and the equilibrium constants are as follows. IL-4 binds with high affinity to IL-4Rα. Thus, IL-4 saturates its binding chain at relatively low cytokine concentration. However, the IL-4–IL-4Rα complex binds with low affinity to either γc or IL-13Rα1. This effectively means that the number of signaling receptors formed (i.e., the ligand–ligand receptor–second chain complex) in response to IL-4 will be highly sensitive to the numbers of γc or IL-13Rα1 chains. However, raising IL-4 concentrations will have very little effect. For IL-13, the situation is fundamentally different. IL-13 binds its ligand-binding chain with low affinity, and therefore the saturation of binding chains is not achieved at low concentrations of cytokine. Thus, the amount of bound IL-13 increases as the cytokine concentration increases. However, the cytokine–binding chain complex binds to IL-4Rα with high efficiency so that the proportion of bound ligand–binding chains that are assembled into signaling chains is high, and the number of signaling chains continues to rise as ligand concentration increases, until most IL-4Rα chains are bound.
Based on our data and the aforementioned binding constants, we wrote a Matlab script to predict the receptor chain assemblage (for details see Materials and methods). For BMDMs (Fig. 7 A), where there are substantial numbers of IL-4Rα chains and of γc chains, but limiting amounts of IL-13Rα1, the prediction is that IL-4 responses are good because large numbers of IL-4–IL-4Rα complexes are formed and there is sufficient γc to drive a reasonable proportion of these into signaling chains. When γc is not present, the concentration of IL-13Rα1 is so low that the number of signaling complexes formed is greatly reduced. In addition, the number of signaling complexes formed is substantially less than the number of IL-13Rα1 chains present because they are recruited to the IL-4–IL-4Rα complex relatively inefficiently. However, the number of signaling chains that can be formed in response to IL-13 can approach the number of IL-13Rα1 chains if sufficient IL-13 is used because the recruitment of IL-4Rα to the IL-13–IL-13Rα1 complex is efficient. Thus, the γc−/− cells respond poorly to IL-4, but can respond quite well to relatively high concentrations of IL-13.
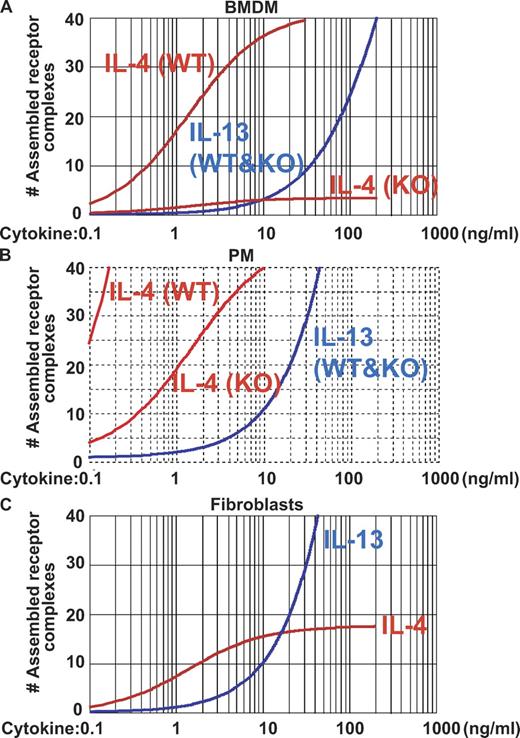
Estimation of the ability of IL-4 and -13 to assemble receptor complexes. (A) Calculated prediction of the capacity of IL-4 or -13 to assemble receptor complexes in BMDMs. The calculation takes into account three major parameters in receptor chain assemblage namely; the estimated receptor chain expression; the known primary binding efficiency of cytokine/cytokine binding receptor chain and the estimated secondary binding efficiency of cytokine/cytokine binding receptor to the second receptor chain (see text for detailed values). (B) Calculation for predicted assemblages of receptor complexes was performed as in Fig. 7 A, using 2.6-fold more IL-4Rα, 4-fold more γc, and 2.5-fold more IL-13Rα1, based on our results shown in Fig. 6. (C) In NIH3T3, expression of γc is very low or nonexisting (Fig. S3). The calculation was performed as above including only IL-4Rα and IL-13Rα1 expression in the analysis. Fig. S3.
Estimation of the ability of IL-4 and -13 to assemble receptor complexes. (A) Calculated prediction of the capacity of IL-4 or -13 to assemble receptor complexes in BMDMs. The calculation takes into account three major parameters in receptor chain assemblage namely; the estimated receptor chain expression; the known primary binding efficiency of cytokine/cytokine binding receptor chain and the estimated secondary binding efficiency of cytokine/cytokine binding receptor to the second receptor chain (see text for detailed values). (B) Calculation for predicted assemblages of receptor complexes was performed as in Fig. 7 A, using 2.6-fold more IL-4Rα, 4-fold more γc, and 2.5-fold more IL-13Rα1, based on our results shown in Fig. 6. (C) In NIH3T3, expression of γc is very low or nonexisting (Fig. S3). The calculation was performed as above including only IL-4Rα and IL-13Rα1 expression in the analysis. Fig. S3.
In PMs (Fig. 7 B), IL-13Rα1 levels are 2.5-fold higher than in BMDMs. This results in a greater sensitivity of the cells to IL-13 because adequate numbers of IL-13–IL-13Rα1 complexes can be assembled at a relatively low cytokine concentration and these efficiently recruit IL-4Rα. Responses to IL-4 in PMs are also obtained at lower concentration because of the increased amounts of γc and of IL-13Rα1. Indeed, because of the increase in the amount of IL-13Rα1, the loss of γc has modest effect on the IL-4 response.
Maximal responses to IL-4 and -13 are achieved with concentrations of cytokine (100 ng/ml or less) that, according to the model, would form 35–40 signaling complexes. Concentrations of IL-13 >100 ng/ml fail to cause greater responses, despite the fact that they would assemble substantially more signaling complexes. However, it is possible that much larger increases in cytokine concentration might lead to increased responses, possibly by recruiting new signaling intermediates.
The model indicates that in BMDMs, 15 signaling complexes are formed in response to 0.1–1 ng/ml IL-4 and to ∼100 ng/ml IL-13, but no concentration of IL-4 achieves 15 signaling complexes in γc−/− cells. In contrast, in PMs, >15 signaling complexes are formed in response to 0.1 ng/ml IL-4 and to slightly more than 10 ng/ml of IL-13. Deleting γc increases the required concentration of IL-4 to form 15 signaling complexes ∼10-fold, but 1 ng/ml is still sufficient to achieve this number.
Discussion
The role of the Th2 cytokines IL-4 and -13 during parasite infections and allergic inflammatory conditions is well established (3, 37). Although most results suggest that IL-4 plays its major role in determining the character of the immune response that will occur, and IL-13 is the major mediator of allergic inflammation, relatively little is known about the comparative potencies of these cytokines on various cell types.
The recently published crystal structures of IL-4–IL-4Rα with γc and with IL-13Rα1, and of IL-13–IL-13Rα1 with IL-4Rα, provides valuable information about these interactions (28). The unique top-mounted, Ig-like domain in the extracellular portion of IL-13Rα1 appears to play an important role in dictating the efficiency of the binding of the IL-13–IL-13Rα1 binary complex to IL-4Rα and the relatively weak binding of the IL-4–IL-4Rα binary complex to IL-13Rα1. The former binding event has a solution KA of 0.5 × 108 M−1 and the latter a KA 2.106 M−1, indicating that the exact same receptor chains, assembled in reversed order by different “driver” cytokines, behave very differently. This thermodynamic data, together with previous solution measurements of the binding affinities, form the basis of our model to explain how IL-4 and -13 can bind to cells with the same receptors in such a manner that the relative abundance of the two receptors determines the relative sensitivity to these two cytokines.
The type II IL-4 receptor is ubiquitously expressed, whereas the type I IL-4 receptor is mainly restricted to hematopoietic cells. Because mouse lymphocytes do not express IL-13Rα1, macrophages are among the few cell types expressing both type I and II IL-4 receptors that offer an easily accessible model to study IL-4– and IL-13–induced signaling via both types of IL-4 receptors. Furthermore, as lack of γc does not interfere with macrophage development (20), the role of the type I IL-4 receptor in different macrophage populations is easy to address. We also tested responses of mouse fibroblasts and human airway epithelial cells, two nonhematopoietic cell types that are thought to express only type II receptors. We limited ourselves to studying the effect of IL-4 and -13 on Stat6 activation and Stat6-mediated gene expression. However, it is of interest to note that IL-4 is reported to be superior to IL-13 in its ability to activate IRS-2 in a γc-dependent manner at IL-4 and -13 concentrations that induce full Stat6 activation (unpublished data).
As we were finalizing this study, it was shown, using PMs and BMDMs from IL-13Rα1−/− mice, that alternative macrophage activation in vivo does not absolutely require IL-13 (8). In line with these findings, we show that Arg1 expression is up-regulated more strongly by IL-4 than by IL-13 in WT BMDMs. Furthermore, we observed a pattern of enhanced IL-4 and -13 responsiveness in PMs. Taking into account the different cell types used here, comparison of IL-4 and -13 responses revealed that relatively immature macrophages (monocytes and BMDMs) rely heavily on the type I receptor; this leads to their relative insensitivity to IL-13. More mature tissue macrophages (PMs) are still extremely sensitive to IL-4, but the lack of type I receptor expression has only a modest effect on IL-4 responses. This suggests that PMs have an additional mechanism to maintain IL-4 signaling that the BMDMs do not. It was obvious that the degree of IL-13Rα1 expression could explain this difference. Indeed, IL-13Rα1 expression was elevated in PMs.
Human monocytes consist of at least two subpopulations, namely CD14hi/CD16lo and CD14lo/CD16hi cells. Although there is still controversy regarding the functional properties of these cells, based on the ability to transmigrate through normal endothelium, CD14hi/CD16lo cells are believed to be inflammatory, whereas CD14lo/CD16hi cells are “residential” monocytes, feeding into the residential pool of macrophages (26). The sensitivity of CD14hi/CD16lo cells toward both IL-4 and -13 was elevated compared with CD14lo/CD16hi cells. In fact, the phosphorylation patterns of Y641 of Stat6 were strikingly similar between mouse BMDMs and human CD14lo/CD16hi monocytes, whereas mouse PMs and human CD14hi/CD16lo monocytes resembled each other. Despite our observation that blocking γc rendered human monocytes from apparently healthy donors unresponsive to IL-4, it is of note that monocytes from a severe combined immunodeficiency disease (SCID) patient with dysfunctional Jak3 kinase responded to IL-4 and -13 with relatively similar potency (38). Therefore, it would be of great interest to study in detail the level of IL-13Rα1 expression in monocytes from this patient because this patient might have elevated expression of IL-13Rα1 to compensate for dysfunctional type I IL-4R signaling, which may explain the discrepancy with our findings.
Because IL-13Rα1–deficient mice show exacerbated Th2 responses during parasite infections, it has been suggested that the type II IL-4 receptor plays an inhibitory role in Th2 responses in vivo (8). However, it can also be argued that the inability of IL-13Rα1−/− mice to expel Nippostrongylus brasiliensis parasites subject the mice to a more prolonged antigenic stimulus, thus enhancing the Th2 response, similar to what is observed in IL-13–deficient mice that are also incapable of expelling the parasite despite a robust Th2-cytokine response (39).
IL-13Rα2 has been proposed to be a decoy receptor for IL-13; it binds IL-13 with high affinity (40). Despite persistent efforts, we did not detect any IL-13Rα2 RNA expression in BMDMs, PMs, or NIH3T3 cells (unpublished data), indicating that the observed differences in the strength of IL-13–induced signaling in BMDMs versus PMs is not caused by expression of an inhibitory IL-13 receptor.
In NIH3T3 fibroblasts, IL-13 was superior to IL-4 in inducing Stat6 phosphorylation. IL-4 and -13 induced comparable degrees of Stat6 phosphorylation in a human lung epithelial cell-line (H292). Together with the observations that larger amounts of IL-13 than -4 are produced in Th2 responses, the relative abundance of IL-4Rα and -13Rα1 explains the central role played by IL-13 rather than IL-4 in mediating effector functions by nonhematopoietic cells (9–11).
We have presented a model that accounts for the differences in potency in these various cell types based on the relative expression of the three receptor chains and on the relative affinities of these chains for their ligands. The basic differences in the “logic” of responses to IL-4 and -13 is that IL-4 binds to IL-4Rα with very high affinity, allowing it to capture cytokines at a very low concentration. However, the construction of the signaling complex is relatively inefficient because the affinity of the IL-4–IL-4Rα complex for either γc or IL-13Rα1 is quite low, so when these chains are limiting, IL-4 responses are severely blunted. In contrast, IL-13Rα1 binds IL-13 with low efficiency. High concentrations of IL-13 are required to assemble the IL-13–IL-13Rα1 complex, but the subsequent step, the binding of IL-4Rα, is relatively efficient so that one can assemble large numbers of signaling complexes if one uses sufficiently large amounts of IL-13. It should be pointed out that other, more complex, models are possible, particularly if multimers of the signaling complex form and if these forms have distinctive signaling capabilities.
What might be the reason for having two functionally overlapping cytokine receptors? As noted, IL-4 is essential for immunoglobulin class switching and for Th2 differentiation. This is easily explained because, in the mouse, IL-13Rα1 is not expressed on lymphocytes, and thus such cells cannot bind IL-13. In contrast, IL-13 is the key effector cytokine. Blocking of IL-13, but not IL-4, can inhibit airway hypersensitivity responses in mice (9–11). IL-13, but not IL-4, is essential for expulsion of parasites in N. brasiliensis infection (8, 39). These findings can be explained both by the equal or greater potency of IL-13 on nonhematopoietic cells and the larger amounts of IL-13 produced in allergic inflammatory responses that may be sustained (or produced) longer than IL-4 at the site of the inflammation (41). Serum IL-13 concentrations during allergic inflammatory responses are often detectable, whereas IL-4 can rarely be found in measurable amounts. For example, in a comparison of atopic patients' PBMC responses to mite allergen, the level of IL-13 was ∼28 times higher than IL-4 in cell culture supernatant (42). In another study, PBMCs from healthy donors that were stimulated for 48 h with anti-CD3 mAb expressed ∼10-fold more IL-13 than -4, as measured by ELISA from supernatants (43). It is also interesting that short-term administration (3 d) of IL-4 to B6 mice results in far greater toxicity than does the same or even larger amounts of IL-13 (unpublished data).
In contrast to the tuning mechanism used to control relative sensitivity in the IL-4–IL-13 system when only IL-4Rα and IL-13Rα1 are available, other cytokine systems with a common signaling mechanism regulate their sensitivity to distinct ligands by controlling the expression of a key binding chain. In the IL-3 cytokine family, the expression of specific α-chain (IL-3Rα-, IL-5Rα-, or GM-CSFRα-chain) triggers heterodimerization to a common β-chain, which initiates signaling. Thus, myeloid cells regulate their responsiveness to these cytokines by controlling expression of the α-chains (44). In the case of IL-2 and -15, which both use the IL-2Rβ–IL-2Rγ complex, specificity depends on the expression of IL-2Rα or IL-15Rα (45), and for IL-7 and TSLP, which share the IL-7Rα chain, specificity depends on the relative expression of γc and TSLPR (46). In this respect, the IL-4–IL-13 system displays a novel mechanism to tune the responsiveness of different cell types to these two cytokines that are structurally analogous, but functionally quite distinct.
Collectively, these observations and the results presented here are consistent with the following scenario. During Th2 responses, early low-concentration IL-4 production can elicit effective Th2-type monocyte responses. As inflammation persists, IL-13 production increases, and the concentration of IL-13 in serum become such that it can also induce efficient responses by both hematopoietic and nonhematopoietic cells. The high degree of toxicity of IL-4 compared with IL-13 may explain why IL-4 concentrations are held at low levels, whereas IL-13 can be produced in larger amounts. IL-13's equal or greater stimulatory capacity for nonhematopoietic cells makes it the dominant effector cytokine.
Materials And Methods
Mice and cell cultures.
Wild type, γc−/−, and Stat6 −/− C57BL/6J mice were obtained from The Jackson Laboratory. Jak3−/− mice (47) were provided by J. O'Shea (National Institute of Arthritis and Musculoskeletal and Skin Diseases, National Institutes of Health, Bethesda, MD). Mice were maintained in the National Institute of Allergy and Infectious Diseases specific pathogen–free animal facility, and the experiments were done under an approved protocol according to the National Institute of Allergy and Infectious Diseases guidelines for animal care. For obtaining BMDMs and PMs, previously described methods were used (48). BMDMs were differentiated in eMEM media containing 10% FBS, penicillin/streptomycin, 2 mM l-glutamine, 0.02% sodium bicarbonate, and 30 ng/ml M-CSF (R&D Systems). Typically, >95% of cells in BMDM cultures were positive for CD11b and F4/80 surface markers after 8-10 d. Before stimulating the BMDMs with cytokines, the cells were starved in growth media containing 2% FBS without M-CSF. After flushing of the peritoneal cavities, PMs were cultured overnight in RPMI containing 2% fetal bovine serum, glutamine, 10 mM Hepes, penicillin/streptomycin, 50 μM 2-mercaptoethanol, and nonessential amino acids. In a typical experiment, cultured cells were 80–90% positive for CD11b and F4/80. Both BMDMs and PMs were cultured on non–tissue culture–treated plates to alleviate the mechanical detachment of the cells from the plates. NIH3T3 and H292 cells were obtained from American Type Culture Collection and were grown in the same media as PMs with 10% FBS. Elutriated human monocytes were obtained from NIH Blood Bank; they were cultured in RPMI containing 2% FBS for 2 h before stimulation with human IL-4 (R&D Systems and Peprotech) or human IL-13 (R&D Systems and Peprotech). All cells were maintained at 37°C with 5% CO2.
Antibodies.
For Western blotting, anti-pStat6 and -Stat6 antibodies obtained from Cell Signaling Technology and Epitomics were used. For mice, antibodies used for flow cytometry were as follows: pStat6, γc, IL-4Rα, CD11b, F4/80 (BD Biosciences). For human cells, antibodies used for flow cytometry were as follows: CD3, CD14, CD16, CD56, CD124, CD132, pStat6 (BD Biosciences), CD19 (eBioscience), and IL-13Rα2 (Diaclone). IL-13Rα1 on human cells was measured with biotinylated polyclonal anti–IL-13Rα1 antibody (R&D Systems). Blocking antibody against IL-4Rα-chain (M1) has been previously described (49); γc blocking antibody was obtained from R&D Systems. Western blot analysis of murine IL-13Rα1 expression was performed with polyclonal anti–IL-13Rα1 antibody from Santa Cruz Biotechnology. Western blot analysis of murine IL-13Rα2 was performed with monoclonal anti–mouse IL-13Rα2 antibody (R&D Systems). Anti-actin antibody was purchased from Santa Cruz Biotechnology.
RT-PCR.
Total RNA was isolated from stimulated cells by using RNeasy kit (QIAGEN) according to the manufacturer's instructions. Equal amounts of total RNA were reverse-transcribed to cDNA using SuperScript II First-Strand Synthesis System for RT-PCR (Invitrogen). Quantitative PCR reactions were performed using a 7900HT sequence detection system (Applied Biosystems). The primer/probe sets for detection of Arg1, IL-4Rα, IL-13Rα1, γc-chain, IL-13Rα2 (FAM-MGB probe), and TaqMan Ribosomal RNA Control Reagents for detecting the 18S ribosomal RNA (VIC-MGB probe) were purchased from Applied Biosystems. The mRNA levels of assayed genes were normalized to 18S ribosomal RNA.
Electrophoretic mobility shift assay.
Nuclear protein extracts were prepared from cytokine-treated cells using a modification (50) of the original method (51). A double-stranded oligonucleotide probe (SBE1) based on a DNA sequence present in the promoter of the human IL-1ra gene was used as a probe in the gel-shift assays (52). This oligonucleotide contains an N4-type GAS element that preferentially binds Stat6, but not Stat1. Binding reactions were performed as previously described (53). A portion of each binding reaction mixture (8 μl per sample) was electrophoresed on nondenaturing, 6% polyacrylamide gels (Invitrogen) using 0.25x Tris-borate-ethylenediamine-N,N,N′,N′-tetraacetic acid buffer (22 mM Tris-HCl, pH 8.0, 22 mM borate, and 0.5 mM ethylenediamine-N,N,N′,N′-tetraacetic acid). The gels were subsequently dried and visualized by autoradiography.
Western blotting.
2 × 105 BMDM or PM cells were lysed in Triton lysis buffer. 150 μg of the total cell lysate from BMDMs and PMs were separated on 12% PAGE-gel, followed by Western blotting and probing of the filter with IL-13Rα1 antibody (Santa Crutz Biotechnology). Detection was performed using SuperSignal West Dura Extended Duration Substrate-kit (Thermo Fisher Scientific) according to the manufacturer's instructions, and equal loading was confirmed either with Ponceau S staining or by reprobing the filter with antibody against actin.
Flow cytometry.
Cell surface markers were stained with the aforementioned antibodies after washing with FACS buffer (1X PBS, 0.1% BSA). For pStat6 intracellular stainings, cells were fixed with 4% paraformaldehyde, and permeabilized with ice-cold 90% methanol followed by staining for 30 min at RT, after which cells were washed and analyzed with FACSCalibur. For each different cell type, the specificity of pStat6 antibody was verified by using unspecific isotype control. No shift compared with unstimulated cells was detected upon IL-4 or -13 stimulation at 100 ng/ml with isotype control in any cell type.
Statistical analysis.
All error bars on graphs show ± the SEM, except in Fig. 3 B, where only + SEM is shown to make the figure more easy to read. All P values were calculated using unpaired Student's t test.
Mathematical modeling.
We used Matlab to calculate the fraction of receptors (IL-4Rα) bound to both cytokine (IL-4 or IL-13) and the second receptor chain (γc or IL-13Rα1 for IL-4 binding and only IL-13Rα1 for IL-13 binding, respectively) as a function of cytokine concentration. Detailed script is provided in Fig. S4 . For a simple receptor (R) – ligand (L) binding at equilibrium, the concentration of the ligated receptor, [R:L] divided by the product of the concentrations of the free receptor [R] and of the ligand [L] is equal to the association constant KA for the reaction:
Because the total concentration of receptors [R0] equals the sum of the concentrations of free [R] and the ligated receptors [R:L], we can replace [R] by [R0] – [R:L] to obtain the fraction of ligated receptors as a function of the ligand concentration [L] and the association constant KA:
For the two-step binding of IL-4 or IL-13 to IL-4Rα, and then to γc or IL-13Rα1, we first calculated the fraction of cytokine-bound IL-4Rα chains and then analogously the fraction of these that are also bound to γc or IL-13Rα1. The second step is a two-dimensional binding process and is treated using two-dimensional concentrations (number of receptors per membrane area) and two-dimensional association constants. IL-13 binding is treated analogously, except for the fact that the second step involves binding to only one possible binding partner, IL-4Rα.
Online supplemental materials.
Figs. S1 and S2 show tyrosine phosphorylation of Stat6 in response to IL-4 and -13 in WT mouse BMDMs and H292 human airway epithelial cells. Fig. S3 indicates IL-4Rα, γc, IL-13Rα1, and IL-13Rα2 expression in NIH3T3 cells. Fig. S4 provides the Matlab script used to calculate receptor complex assemblage.
Acknowledgments
The authors wish to thank the Cytokine Biology Unit for support. We especially acknowledge Drs. L. Guo, R. Yagi, and J. Zhu for valuable comments and Dr. J.D. Milner for sharing unpublished results with us. J. Hu-Li, C. Watson, and X. Chen are thanked for excellent technical assistance. Drs. N. Heller, X. Qi, K.A. Shirey, S.N. Vogel, and A.D. Keegan are thanked for sharing unpublished results with us. Dr. M. Janka-Junttila shared valuable technical assistance with work on human monocytes. Shirley Starnes is thanked for editorial assistance.
This work was supported by National Institute for Allergy and Infectious Diseases Intramural Program, the Finnish Cultural Foundation, the Finnish Medical Foundation, and the Emil Aaltonen Foundation.
The authors have no conflicting financial interests.
References
Abbreviations used: Arg, Arginase; BMDM, BM-derived macrophage; EMSA, electrophoretic mobility shift assay; γc, IL-2 receptor-γ chain; IRS, insulin receptor substrate; MFI, median fluorescence intensity; PM, peritoneal macrophage; Tg, thioglycollate; TLR, Toll-like receptor.